- Reference Number: HEY428/2026
- Departments: Tissue Viability
- Last Updated: 31 January 2026
Introduction
This leaflet has been produced to give you general information about your assessment and treatment to prevent and treat pressure ulcers.
It is not intended to replace the discussion between you and your nursing staff but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for you.
To help prevent pressure ulcers it is important that we work together to prevent unnecessary deterioration of your or your friend/ relative’s skin. This information leaflet is designed to help you understand all your individual risk factors and balance the risk of declining skin inspections and risks to you developing pressure ulcers.
Humber Health Partnership use the ASSKING framework –which is a nationally recognised tool used for the prevention and treatment pressure ulcers.
A-Assessment
S-skin inspection
S-surface selection-mattress or seat cushion
K-keep moving
I-Incontinence management
N-Nutrition
G-Give information
What is a pressure ulcer?
A pressure ulcer is an area of damage to the skin and/or underlying tissue, commonly known as ‘bed sores’. They are usually caused by sitting or lying in one position without moving for a period of time. A pressure ulcer can develop very quickly, even in a few hours, especially if you are unwell or have certain illnesses.
Pain may be one of the first signs that a pressure ulcer may be developing and your skin will start to change colour. It may appear slightly red or darker in colour than usual and does not fade when pressure is removed. In some cases, it can appear purple /maroon in colour and can initially be mistaken as a bruise. Part of the assessments the healthcare professional caring for you undertake involves looking closely at your skin to detect these changes.
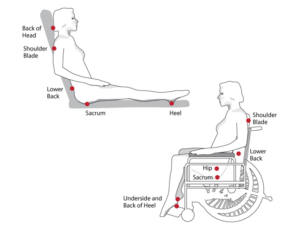
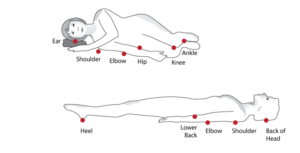
In people who have darker skin tones it is not easy to detect a reddened /purple area. In this case, it is best to check by touching the areas of the body that are at risk from pressure ulcers –see diagram below. These areas may feel warmer or cooler to touch, firmer, spongy or swollen.
Your help in detecting the early signs of skin damage is important, by alerting our staff to any concerns can help prevent pressure ulcers developing or getting worse.
If the early signs of a pressure ulcer are not treated quickly, it can develop into an open wound, which can lead to a more serious pressure ulcer
If you already have early signs of a pressure ulcer or have one already when you are admitted, you will be provided with the appropriate pressure relieving mattress. Within our trust we have different types of mattresses and cushions which will help reduce the pressure on your skin. All our foam mattresses are made of high-quality foam but if you need a more specialised air mattress or cushion, the staff will assess you for this. These will move slightly when you are laid on them to relieve the pressure, but please ask the staff to explain them to you.
Self- care
- Keep your skin clean and dry, including under your breasts, in between the cheeks of your bottom, under your scrotum.
- Moisturise your skin.
- Your pressure ulcer may need other treatments to help it to heal. This could include dressings and referrals to other health professionals.
- Ask your health care professional if you are unsure of any aspect of this care
Are you at risk of developing a Pressure ulcer?
Anyone can develop a pressure ulcer but some people are more likely to develop a pressure ulcer than others.
Part of the risk assessment involves looking closely at your skin to detect early changes that may indicate damage may be developing. Your nursing team will ask your permission to assess and plan any care required.
You are at risk of developing a pressure ulcer if you:
- Are not eating a balanced diet or having enough to drink
- Have to stay in bed for a period of time
- Have problems moving position without help
- Are in a wheelchair
- Spend a long time in an armchair or on a sofa
- Are seriously ill (even for a short period of time)
- Are undergoing surgery
- Are incontinent
- Have lost your feeling in part(s) of your body (e.g. after a stroke or spinal cord damage)
- Have poor circulation
- Have previously had a pressure ulcer
- Pain preventing movement / hindering repositioning
- Have a medical device in place
- If you are taking multiple medications
- Unwell and less mobile requiring hospital admission
- Pressure ulcers can also develop very quickly in the elderly population.
Pressure ulcers can be painful, and you are more likely to develop an infection which can then make you seriously ill. They can take a very long time to heal and can delay your discharge home. This will allow us to monitor if it is improving or getting worse, in which case we will suggest a change in turns, a di
If you are in bed:
- Change your position and regularly alternate between laying on your back and sides. This may be difficult for you to do on your own and a nurse will help you. It is important that you remind your nursing team that you need to be repositioned if the time you were due has passed. Please help us by you or your carer reminding us that you need to be turned.
- If you have red/blistered heels we may need to raise your feet off the bed.
- If you are sitting out of bed but cannot move yourself around or stand up, it is important that you do not sit out of bed for long periods of time without standing up regularly. Our staff will assist you if you need help to get back into bed.
If you are in a wheelchair:
- Try to take your weight off your bottom every half an hour by leaning to one side or pushing up on the arms of your chair.
- Regularly roll from buttock to buttock a few times every half an hour.
- You should not sit in your wheelchair for more than three hours at a time, even with a specialised cushion.
What else can you do to help prevent pressure ulcers?
Eat a healthy diet and drink plenty of fluids, if this is possible. We may refer you to a dietician and provide supplements.
Inform our staff of any equipment to prevent or treat pressure ulcers you already use.
Inform our staff if you are not happy with the equipment
Which areas of skin are most at risk?
The common places for pressure ulcers to occur are on parts of the body that take your weight and where bone is near to the surface of the skin. For example, bottom, heels, hips, elbows, ankles, shoulders, spine and the back of the head.
Devices in use to support your care may also cause damage to the skin from pressure if not repositioned regularly.
If you have any questions regarding your pressure ulcer risk, care planned or equipment used please ask your health care professional.
To ensure your care is planned as required the nursing staff will seek your permission to check your skin to ensure no damage has developed or that your skin is not more vulnerable than usual. This leaflet is aimed at providing you with the information to support why this is necessary.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

