- Reference Number: HEY1406/2024
- Departments: Paediatrics
- Last Updated: 29 February 2024
Introduction
This leaflet has been produced to give you general information. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and the healthcare team, but may act as a starting point for discussion. If after reading it, you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
Urticaria
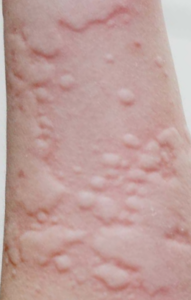
Is a common skin condition characterised by recurrent, transient, raised and itchy (not usually painful) lesions. Lesions are often called hives, weals/wheals or nettle rash. Urticarial wheals can vary in size from the size of a pinpoint to several centimetres in diameter. They can be either localised or widespread.
Angioedema
Is swelling, often involves the eyelids, tongue and lips. Angioedema is often tender or painful rather than itchy. The resolution is slower than for urticarial and can take up to 72 hours.
How is urticaria in children classified?
- Urticaria in children can be either acute (episode often gone within hours to days) or chronic (urticaria occurs most days for more than 6 weeks).
- In both the acute and chronic urticaria, the individual spots last less than 24 hours.
- Children with acute urticaria may also have angioedema.
- Urticaria (acute, intermittent and chronic) affects around 3.4% of British children.
What is the cause?
The rash and swelling is cause by substances such as histamine being released from cells in the skin called mast cells. The same thing happens in the skin in food or venom allergies, so this is why the rash looks the same.
Triggers:
- In most children with recurrent or chronic (urticaria and/or angioedema) there is no clear trigger for this to occur. This is called ‘idiopathic’ or ‘spontaneous’ urticarial.
- Many episodes of urticaria in childhood are caused by virus infection. Sometimes it is due to other infections such as respiratory (Mycoplasma, streptococcus), dental and urine infections which may need antibiotic treatment.
- Contact and irritants (e.g. to plants, animals or latex).
- Cold urticaria. Triggered by exposure to cold, including rain, cold wind and cold water. Swimming in cold water may cause severe whealing and fainting and should be avoided.
- Delayed pressure urticaria. Urticaria develops where pressure has been applied to the skin, for example from tight clothes or from gripping tools. Usually the swelling develops several hours later. It can be painful and last longer than a day.
- Scratching, rubbing.
- Solar urticaria. This is rare. Occurs immediately after exposure to sunlight, and last for less than one hour after avoidance of exposure.
- Cholinergic urticaria. This occurs under conditions that cause sweating, such as exertion, heat, emotional stress and eating spicy food. Within minutes. The wheals last for less than an hour, but in severe cases may join together to form larger swellings. Antihistamines usually help, and are sometimes best taken before a triggering event (e.g. exercise).
- Aquagenic urticaria. This is extremely rare. Small wheals occur on the skin at the site of contact with water, usually on the upper part of the body.
- Urticaria prior to menstruation.
- Medications particularly ibuprofen and (NSAIDS) or some blood pressure medications.
- Recurrent urticaria can occasionally be linked with abnormal thyroid gland function or coeliac disease.
- Angioedema is often idiopathic. Similar to Urticaria, viral infections are a common cause in the paediatric population.
- If there is only angioedema with no Urticaria, tests for a rare illness called hereditary angioedema may be required.
Is urticaria and angioedema an allergy?
A single episode of urticaria or angioedema may be due to an allergy but unless there is an obvious link with a particular food or pollen allergy is not usually the cause. If the urticaria does not clearly follow within about one hour of eating a food, it is very unlikely to be caused by that food.
Is recurrent urticaria and angioedema life-threatening?
It is extremely unlikely for recurrent or chronic urticaria to be life threatening. The tongue and lips may swell which can be alarming but is harmless and does not usually result in breathing problems. If however you have any difficulty breathing during an attack, call an ambulance.
How long will the urticaria and angioedema continue?
It is not a severe disease and it remits over time. A quarter of children with chronic spontaneous urticaria are disease-free 3 years after presentation and 96 per cent are asymptomatic after 7 years.
What is the treatment?
- The most commonly used medications for urticaria and angioedema are antihistamines. These can be used at the start of an attack to reduce the itching, rash and swelling.
- If the urticaria or angioedema occurs frequently then antihistamines are best taken every day to prevent attacks. For those with recurrent urticarial and angioedema antihistamines can be safely taken for prolonged periods of months or even years.
- The newer non-sedating antihistamines such as cetirizine, loratadine and fexofenadine are preferred to the older antihistamines such as chlorphenamine (Piriton®) as they are more effective and the older types can make children drowsy and affect concentration.
- Different people will do best on different antihistamines so if the first one tried is not helpful then another antihistamine should be tried.
- If there is not any urticaria or angioedema for several weeks when taking antihistamines then it is worth stopping the medication to see if they are still needed. If the urticaria/angioedema returns, the antihistamine should be restarted.
- Occasionally other medications are needed if the episodes do not improve with regular antihistamines. These medications include leukotriene receptor antagonists.
- Prednisolone (an oral steroid) is occasionally used for severe attacks but cannot be used frequently or for prolonged periods.
- If an antihistamine is required in pregnancy, the lowest dose of cetirizine or loratadine should be used.
- Cetirizine is licensed for the treatment of chronic urticaria in children from one year of age; loratadine is licensed for the treatment of children of 2 years and older. Fexofenadine is licensed for use in children over 12 years.
Key Points
- There are many causes for urticaria, most are idiopathic or viral.
- If urticaria occurs with involvement of other symptoms (e.g. persistent cough, hoarse voice, difficulty swallowing, difficult or noisy breathing, persistent dizziness, pale or floppy, (collapse/unconscious), anaphylaxis should be suspected. Urgent administration of adrenaline and medical assessment is required.
- If the lesions are painful rather than itchy, last more than 48 hours, leave discolouration on the skin or associated with significant lethargy , stomach pains or joints swelling then seek medical advice from your general practitioner or children emergency departments.
References:
- RCPCH- Allergy Care Pathways for Children Urticaria/Angio-oedema/Mastocytosis.
- Urticaria in children .Dermnet. Topics.
- British Association of Dermatologists leaflet.
- BSACI guideline for the management of chronic urticaria and angioedema.
- https://www.allergyuk.org/
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Paediatric Allergy Nurses on tel: 01482 461403.

