- Reference Number: HEY276/2025
- Departments: Renal Service
- Last Updated: 31 December 2025
Introduction
This leaflet has been produced to give you general information about your procedure. Most of your questions should have been answered by this leaflet. It is not intended to replace the discussion between you and your doctor but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
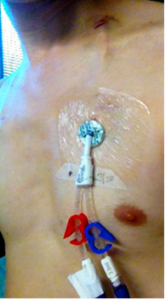
By General Ludd – Own work, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=27359127
Why do I need a Tunnelled Haemodialysis Line?
The tunnelled dialysis line is used to connect you to a haemodialysis machine. The machine removes the waste products and excess fluid that the kidneys cannot remove. This is required because your kidneys are damaged to the extent that they need the machine to take over their normal function.
The tunnelled line can be kept in for several weeks or months until a more permanent access like a fistula is created.
How do I prepare for the Tunnelled Haemodialysis Line Insertion?
Please read this information leaflet. Share the information it contains with your partner, family or friends (if you wish) so that they can be of help and support. There may be information they need to know, especially if they are taking care of you following this examination.
If you are on blood thinning medications like warfarin, aspirin or clopidogrel, please inform your doctor. You will be informed by the doctor or the renal access nurse if you need to stop any of these medications before the procedure. You will always be asked to sign a consent form prior to the procedure. This confirms that you understand the risks and benefits of the procedure and have given your permission for it to go ahead.
People naturally carry germs (including bacteria) on their skin, which sometimes can cause infections, especially during medical procedures like neckline insertions. To prevent these infections, decolonisation is used. This involves cleaning the skin with antiseptic solutions/ body washes and applying an ointment (cream) inside the nostrils. Patients will be provided with these products prior to the procedure and should continue daily for 5 days after the tunnelled line insertion. If you have not received these, please inform us straight away.
What will happen?
The procedure will usually take place in the procedure room on the Renal Ward at the Hull University Teaching Hospital NHS Trust. You will be asked to lie on your back; the trolley you are lying on may be tilted so that your head is slightly below your feet. As routine, you will be attached to the ECG monitor, (which is a device that monitors heart activity) and a probe will also be placed on your finger to measure oxygen levels and if indicated you may be given oxygen during the procedure.
As this procedure is invasive, the skin over the veins in the neck or groin will be cleaned with antiseptic and sterile drapes will cover the area including your face to keep the area clean. If you think you may be uncomfortable with your face covered, please inform the nurse.
Local anaesthetic will be injected into your skin, which stings a little at first. Once your skin is numb, more local anaesthetic is injected around the vein. The doctor will find the exact position of the vein using an ultrasound scan. You should feel some pressure but should not feel any pain. Please inform the doctor/nurse if you have any pain.
A small cut is made in the skin over the vein. Whilst continuing to monitor the location of the vein, with the ultrasound machine, the doctor will put a special needle through the numb skin into the vein. The doctor will then pass a thin wire through the needle into the vein, and the needle will be removed. The tunnelled line is then placed through the skin and into the vein by passing it over the wire. If it is not a single line, this is repeated twice. Once the dialysis line has been inserted, the wire is removed. The ends of both lines will then be tunnelled under the skin. The line is held in position naturally by the skin with the help of a small cuff at the end of the line, sutures will be used to hold the line in position until the cuff is bedded in fully, these remain in situ for three weeks. Stitches will be used to close the entry site, these remain in situ for seven days and a dressing will be used to cover the other end.
Very rarely, the line may have to be inserted in the groin vein if there are no suitable veins in the neck. The procedure will essentially be the same, and the line will be tunnelled in the thigh.
Can there be any complications or risks?
- Occasionally, it may not be possible to insert the line due to narrowing of your central veins. If this happens, you will have the line inserted in the Radiology department under x-ray guidance
- Infection – either a local infection or a bloodstream infection. This can be treated with antibiotics but sometimes the tunnelled dialysis line has to be removed
- Localised bruising and/or bleeding around the entry site affects one in every 10 patients
- Heart rhythm disturbances: this is due to irritation of the heart muscle from either the guide wire or the central line. This is identified on the ECG monitor, which monitors your heart activity, and will be quickly corrected
- Arterial puncture (catheter in an artery instead of a vein) and incorrect positioning of the catheter, affects one in 100 patients, however this risk is reduced as ultrasound equipment is used to make the insertion more accurate
- During the procedure the lung may be punctured, and you may require further treatment. This is uncommon as ultrasound equipment is used to make the insertion more accurate
What happens after the insertion procedure?
Once the procedure is finished, you will be transferred back to the ward, or if you have come as an out-patient you will just sit quietly on the ward until you go for your chest x-ray. You will have a chest x-ray performed to make sure the line is in the correct position and also to rule out any line related complications. The line site may bleed a little and feel sore. If you notice any bleeding let the nurses know. It is important to make sure that the tunnelled line is always covered with a dressing to prevent infection. You will be given more instructions by the staff nurse about caring for your line once it has been inserted. You may be allowed to go home once the chest x-ray has been reviewed by the doctor and you may wish to take things easy for a day or two. You may be dialysed the same day to ensure the line works well with the dialysis machine.
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Renal Department Tel: 01482 674980.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

