- Reference Number: HEY1083/2019
- Departments: Gynaecology, Radiotherapy
- Last Updated: 31 July 2019
Introduction
This leaflet has been produced to give you general information about external beam radiotherapy to the female pelvis, in addition to the information you will receive from your Clinical Oncologist. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and your doctor, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
What is radiotherapy?
Radiotherapy is the use of high energy X-rays and other types of X-rays (e.g. electrons) to treat cancer. Radiotherapy works by causing chemical and physical damage to the cancer cells in the treatment area. Although some normal healthy cells are also affected during radiotherapy, these are able to recover and repair themselves over time.
Radiotherapy can be used for a number of different intended benefits. For example, radiotherapy can be used as a curative form of treatment following surgery, in combination with chemotherapy, brachytherapy, (internal radiotherapy), or used as symptom control. Radiotherapy does not make you radioactive and you are safe to be around all people including children whilst you are on treatment.
The Clinical Oncology Consultant looking after you will have already discussed the type of treatment(s), you will be having, their side effects and will have gained your consent to proceed with your radiotherapy treatment.
There are several stages prior to you actually commencing your radiotherapy treatment.
The areas being treated
These diagrams may be useful to help you understand where your cancer is and the area to be treated with radiotherapy. It may also explain why we may request you have a full bladder for your radiotherapy planning scan and radiotherapy treatment.
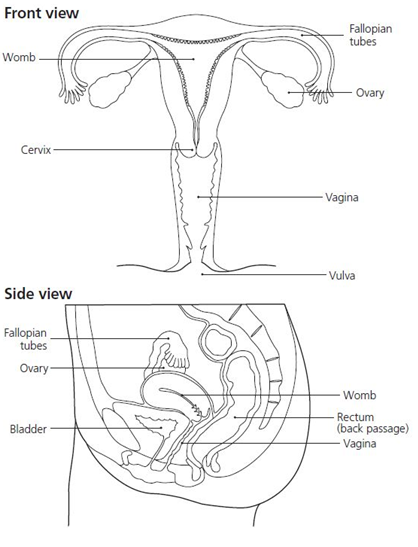 Planning your treatment
Planning your treatment
Your first appointment in the Radiotherapy Department will be a planning appointment. This appointment will be approximately 45 minutes to one hour in duration.
A member of the radiotherapy team will speak to you before any procedure is carried out to obtain your consent for this planning process. For the purposes of the planning scan and treatment thereafter you may be asked to achieve a comfortably full bladder and an empty rectum. A specialist X-ray machine called a CT (Computed Tomography) scanner will be used as part of the planning process. This machine enables us to obtain images of the area of interest whilst you lie on the CT couch. You will move backwards and forwards through the hole of the machine very slowly, pictured, (Fig 2), and you will not feel anything at all.

In the CT room, you will have to loosen or remove your clothing only in the area of interest (i.e. the lower body) and then you will be helped into the correct position on the couch. We will draw some temporary markings onto your pelvis area. The staff will then leave the room to perform the scan. Upon returning, three or four permanent markings (tattoos), will replace the temporary marks; this is done by using a sterile needle and ink. These marks will be the size of a freckle and allow the radiotherapy staff to accurately align and reproduce the correct position daily for treatment.
The information obtained from this scan is used to produce your individual treatment plan. The CT staff will confirm your treatment start date before you leave the department.
After the scan you will meet a member of the patient support team who will talk through the radiotherapy treatment, its possible side effects, how you can help to minimise them and how we can help you. This is also another opportunity for you to ask questions or raise any concerns you may have.
Radiotherapy treatment – what happens on the first day?
On your first day, and each day afterwards, when you attend please book in at the radiotherapy reception desk. You will be asked to take a seat either in the main waiting area or you will be directed to a specific waiting area.
If you had to achieve a comfortably full bladder and an empty rectum for your planning scan you will have to repeat this for all of your radiotherapy treatments. Both these requirements are very important for the accuracy of your treatment.
What happens during treatment?
Radiotherapy is painless and usually takes 10 to 15 minutes to deliver, by a machine called a Linear Accelerator (Fig 3) or Linac, for short.
A member of staff will escort you into the treatment room. A curtained private changing area is available should items of clothing need to be removed, maintaining your privacy at all times.
The radiographers will then assist you into the correct treatment position on the couch. This will be the same position you were in for your CT planning appointment. The radiographers will then move the Linac into position, ready for treatment. The radiographers are controlling the Linac at all times and the machine may seem close to you but it will not touch you. Once you are set up in the correct position, the radiographers will let you know that they are leaving the room and then leave for a few minutes to commence treatment.
The machine is being controlled by the staff outside in the control area and will rotate around you in different directions. The radiographers are watching you at all times on the TV monitors and should you feel you want to stop the treatment at any time just wave to attract their attention. The machine will stop and the radiographers will come back into the room. You will not feel or see anything during your treatment, however, you may hear a buzzing sound when the treatment is being delivered.
Reviews during treatment
You will have regular weekly reviews with a radiographer as you progress through your treatment to assess how you are coping with any side effects and your general well-being. You may be referred to our radiotherapy support team if further medical advice or intervention is required.
If you are to receive Brachytherapy, (internal radiotherapy treatment), after your external beam radiotherapy, your consultant will have already discussed this with you and gained your consent. The Brachytherapy team will meet with you in your last week of external beam radiotherapy and go through the brachytherapy treatment, its possible side effects, and how we can help you. This is also another opportunity for you to ask questions or raise any concerns you may have.
Side effects and treatment
You may experience some side effects and reactions as you progress through your treatment. Every individual is different and as such you may experience some of these and at varying times and levels. This is normal and temporary so please do not worry. You can speak to the radiographers or the support team regarding how you can control them and/or if your symptoms worsen, they can advise and treat you accordingly.
Listed below are some of the most common side effects experienced. These usually begin approximately 2 to 3 weeks into treatment and may continue for a short while after you have completed your radiotherapy but will then slowly settle down.
For those ladies who are also receiving chemotherapy along with radiotherapy, the chemotherapy nurses will discuss the side effects caused by chemotherapy with you.
Early side effects
Radiotherapy treatment will cause some degree of diarrhoea, tiredness and cystitis. These side effects are temporary. For all the side effects let a member of staff looking after you know how you are feeling and they can advise the best way to help or they may refer you to the support team.
Bowel
Your bowels may become altered due to your treatment. For most women, this is in the form of diarrhoea but occasionally it can be constipation. It can start about 10 days into treatment and can last several weeks after the treatment finishes. With diarrhoea patients often get wind, abdominal cramps, bloating and may pass mucus.
Bladder
Radiotherapy can irritate the bladder and give symptoms of cystitis, such as increased frequency, urgency and a burning or stinging sensation when passing urine.
Vaginal discharge or bleeding
You may develop a discharge or light bleeding; this is not unusual but let a member of the team caring for you know for advice. If the discharge or bleeding alters e.g. becomes heavier or smells unpleasant please see the support team.
Haemorrhoids (piles)
If you already suffer with haemorrhoids they may become inflamed due to the increase in bowel motions. Please speak with a member of the support team before using your normal ointment/cream.
Skin Reactions
Sometimes radiotherapy may cause skin in the treated area to become sore or pink, especially around the groin area and in between the buttocks. This is rare and advice will be given on how to care for your skin if this does happen and cream may be supplied. It is also possible you will lose the hair within your pubic region.
Fatigue/Tiredness
Some patients may experience feeling more tired than usual during treatment. This could be due to having to get up several times during the night or travelling a long way for daily treatment. Be sensible and rest when you feel the need to though gentle exercise is also often of benefit. Normal energy levels will return around one month after your treatment has finished.
Nausea
Some ladies may feel sick during their radiotherapy with taste changes or going off your food. This is more likely to happen if you are having chemotherapy.
Long term effects
In pre-menopausal women this treatment will stop the ovaries working causing early menopause.
Radiotherapy carries a small risk of damage to the bladder, bowel, vagina and pelvic bones which can be long term and sometimes requires surgery.
Radiotherapy may cause some narrowing of the vagina which is usually preventable but it can sometimes impact on sexual function.
Post Radiotherapy Treatment
Once you have completed your course of radiotherapy treatment, you will receive a follow-up appointment. This appointment will be sent to you in the post for you to see your Consultant Oncologist again at the hospital where you were first seen. This is usually around 4 to 6 weeks after treatment has finished, as time to allow any side effects experienced to settle down is required. Your Consultant will then decide if any further tests / appointments are necessary.
Advice and Support Services
Please read the information leaflet. Share the information it contains with your partner and family (if you wish) so that they can be of help and support. There may be information they need to know, especially if they are taking care of you following this treatment.
Radiographers
These highly trained specialists help in several aspects of your treatment from CT and treatment. You will see where possible the same team of radiographers each day you attend for your treatment. They are there to help you if you have any problems or worries. Please feel free to speak to them regarding any help and advice. You may be referred to another member of the oncology team as necessary.
Radiotherapy Support Team
The team consists of Registered Nurses and Clinical Support Workers (CSW) who are based within the Radiotherapy Department. They actively support and advise patients receiving radiotherapy treatment. They are able to make appropriate referrals and offer advice to patients and their families/carers.
Health Centre
The primary aim of our Health Centre is to help patients and their families to have the best possible health and quality of life during and after treatment. The Health Centre is open to all oncology patients and their families and offering an informal atmosphere to those who wish to “drop in” to the centre. Specially trained staff are available to advise on different aspects of coping with cancer.
The centre is located in the Main Reception of the Queen’s Centre at Castle Hill Hospital.
Opening times are Monday to Friday 9:00am to 5:00pm
Macmillan Cancer Support
Macmillan Cancer Support provide information from specialist nurses on all aspects of cancer and its treatment and on the practical and emotional aspects of living with cancer.
You can drop into the Macmillan Cancer Information Centre at the Queen’s Centre or call them on tel: 01482 461154 (Monday to Friday 9:00am to 5:00pm)
Alternatively free-phone the national help line tel: 0808 808 0000 (Monday to Friday 9:00am to 8:00pm)
Online: http://www.macmillan.org.uk
Write to: Macmillan Cancer Support, 89 Albert Embankment, London, SE1 7UQ
PALS (Patient Advice and Liaison Service)
Provide confidential advice and supports, helping you resolve any concerns you may have about the care we provide, guiding you through the different services available from the NHS.
Tel: 01482 623065 (Monday to Friday 9:00am to 4:00pm)
Email: hyp-tr.pals.mailbox@nhs.net
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Radiotherapy Information and Support Team on tel: 01482 461206 Email: hyp-tr.radiotherapy.information@nhs.net
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

