- Reference Number: HEY249/2025
- Departments: Orthopaedics, Physiotherapy
- Last Updated: 31 May 2025
Introduction
This leaflet has been produced to give you general information about your condition. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and your doctor but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for you.
What is the Plantar Fascia?
The plantar fascia is a band of thick tissue that runs along the sole of the foot. It runs from the heel bone (calcaneum) along the inside edge of the foot to the base of the toes. Its function is to help lift the arch of the foot when walking and act as a shock absorber for the whole leg.
What is Plantar Fasciitis?
Plantar fasciitis is a condition that causes pain on the bottom of the foot around the heel and arch. The pain occurs when plantar fascia becomes inflamed due to repeated stress. It often develops over time but can occur suddenly.
What causes Plantar Fasciitis?
The cause of plantar fasciitis is not always clear. However, several factors can contribute to the development of plantar fasciitis, including:
- A sudden increase in the amount of activity you do, such as running or walking
- Standing for long periods of time when this is not normal for you
- Being overweight
- Overstretching the sole of the foot
- You have high or low arches of the foot
- Ageing
- Wearing shoes with poor cushioning or poor arch support
- Tightness in the calf muscles
What are the symptoms?
The main symptom of plantar fasciitis is pain. The pain occurs on the bottom of the foot. It is most commonly around the heel but can appear in the arch.
The pain is often worse when you first begin walking after a period of rest where there is no weight on the foot, such as after sleep. Also, after standing, walking or running for a long period of time. It may also be painful to stretch the bottom of your foot.
The pain often eases with gentle exercise such as after you begin walking in the morning.
How is Plantar Fasciitis treated?
Your plantar fasciitis symptoms can improve over time by itself. However, you may choose to follow this advice to try and encourage your recovery and relieve your symptoms. This advice includes:
Rest and Gentle Exercise –
You should rest the foot as much as possible. Avoid running, excessive walking and long periods of standing as these place large amounts of stress on the foot.
However, exercises that place minimal pressure or stress on the feet, such as swimming or cycling, are advised
It is also recommended that you do regular, gentle exercises that stretch the sole of the foot and heel and strengthen the muscles in the foot to reduce the stress on the foot.
Exercises:
- Stand facing a wall and step backwards with your injured leg.
Keep this leg straight with your toes pointing forwards, towards the wall and your heel flat on the floor
Now bend your other knee until you feel a stretch in the calf of your injured leg. Hold this stretch for 30 seconds, repeat 3 times a day.

2. From the position above move your injured leg forward but keep it slightly behind your other leg.
Ensure that your toes stay pointing forwards and bend both knees. Keep the heel of your injured leg on the floor.
You should feel a stretch in the calf of your injured leg. Hold this stretch for 30 seconds, repeat 3 times per day

3. Stand facing a step and place the toes of both feet on to it, letting your heels hang over the edge.
You may need to hold onto something solid for support such as a handrail. Then lower your heels below the step, keeping your knees straight.
You should feel a stretch in your calves. Hold this for 30 seconds, repeat twice when completing these exercises.

4. Sit on a chair with your knees bent at right angles and your feet flat on the floor.
Lift your toes upwards, keeping your heels on the floor. You should feel a stretch along the bottom of your foot.
Hold this stretch for 30 seconds, repeat 3 times every time you complete these exercises.
5. Loop a towel or scarf around the ball of your foot. Use the towel to pull your toes up towards your body, keeping your knee straight.
Hold the stretch for 30 seconds, repeat 3 times every time you complete these exercises.

6. Using a round drinks bottle that has been chilled in the freezer, sit on a chair and place the bottle under the arch of your foot. Roll your foot forwards and backwards over the bottle for five minutes, repeat twice per day.
To ensure that you do not receive a skin burn, please follow the advice in the section below entitled pain relief, regarding the application of ice.
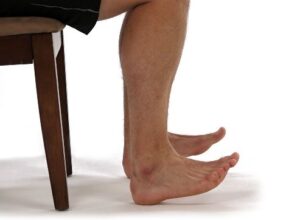
7. If you are able to stand on your toes without pain, you can complete heel raises to strengthen the muscles.
Holding onto a chair, spread your weight evenly between both feet and push up onto your toes as high as possible.
Hold for 5 seconds, then slowly lower down. Repeat this 10 times, 2 times per day.
You can decide to progress this exercise if it feels or becomes easier. You can increase the number of repetitions or you can repeat this exercise stood only on the affected leg. If you complete this exercise on one leg, also complete it on the other leg.

All photos with kind permission of ©Physiotec™
Footwear
You should avoid wearing high heels, tight shoes, flip-flops or backless slippers and walking on hard surfaces in bare feet. Shoes that have good arch support and cushion the heel are recommended. Insoles or heel pads in your shoes may help improve your symptoms.
Pain relief
Ice may help reduce the pain in your foot and so should be applied for 15 – 20 minutes regularly throughout the day. There are many different ways in which ice can be applied. It is believed that crushed ice, in the form of frozen peas for example, is the most effective.
Whichever method you choose it is important that you wrap the ice in a damp towel, in order to prevent it from ‘burning’ the skin.
Please Note:
- Only use an ice pack on areas that have normal skin sensation i.e. where you can feel hot and cold
- Do not apply ice to an open wound
- Do not apply an ice pack to an area that has poor circulation
- When you apply ice to your skin, check the skin every five minutes and stop using it if:
- the area becomes white, blue or blotchy
- the area becomes excessively painful, numb or tingles
Over the counter pain relief, such as paracetamol or ibuprofen gel can also be used. However, before starting any medication please seek advice from your doctor or pharmacist.
When to seek further help
If, despite following the advice above, you are struggling to weight bear without pain you should self-refer to physiotherapy by contacting the following number depending on the location of your doctor:
- Hull GP patients self-refer to Healthshare: (01482) 300003
- East Riding GP patients self-refer to East Riding Physiodirect: (01377) 208300 or self-refer online at chcpmsk.org.uk
This leaflet was produced by the Physiotherapy Department Hull University Teaching Hospitals NHS Trust and will be reviewed in May 2028.

