- Reference Number: HEY1313/2025
- Departments: Respiratory Medicine
- Last Updated: 30 September 2025
Introduction
This booklet has been produced to give you important information to help you care for someone receiving treatment from the Home Ventilation Service. Most of your questions should be answered by this booklet- please keep it in a safe place as you may need to refer back to it in the future. If after reading it you have any concerns or require further explanation, please discuss it with a member of the Home Ventilation team.
What is Home Ventilation
Home Ventilation is also known as assisted mechanical ventilation which is provided in a patient’s own home, Hospice, Nursing or Care home setting. It is a treatment to help with breathing- if breathing becomes difficult or muscles tire it may lead to a buildup of carbon dioxide (hypercapnia) and low levels of oxygen (hypoxia) in the blood. A number of different medical conditions can cause breathing to be reduced or become less regular, especially while sleeping.
This treatment is usually delivered through a face or nasal mask and is referred to as Non- Invasive Ventilation (NIV). In some cases, due to their clinical condition, a patient may have a tracheostomy inserted and ventilation will be given through this route (Invasive Ventilation).
This treatment is not the same as ‘CPAP’ which is commonly used to treat Sleep Apnoea.


Why does the patient need Assisted Mechanical Ventilation?
The patient will have had various tests and investigations performed which will show they have respiratory failure. Their underlying medical condition will have affected their ability to breathe effectively overnight so they do not gain the full benefit of a good night’s sleep. Symptoms you may observe include tiredness during the day, disturbed nighttime sleep, lack of energy and morning headaches-this could be due to lack of sleep but also due to ineffective breathing. If your patient is diagnosed as having respiratory failure it means their lungs cannot breathe out the waste products it needs to- leading to a buildup of Carbon Dioxide. If the level of Carbon Dioxide gets too high, they will become very unwell, and it is potentially life threatening.
By using assisted mechanical ventilation, the patient should have an improved sleep quality leading to better energy and concentration levels during the day. It can make them feel less breathless, so they feel more able to perform daily tasks. They may feel brighter on waking and be headache free. Ventilation can also reduce the likelihood of them getting chest infections requiring admission to hospital for treatment.
If the patient requires admission to hospital, please ensure they take the ventilator and patient booklet to hospital with them- they must continue with this treatment in hospital. Some areas of the hospital and some nursing and/or medical staff may be less familiar with this equipment- please ask them to contact the Home Ventilation Team as soon as possible for support and advice. Please inform us if your patient has been admitted so that we can review in hospital- there is a 24-hour answerphone available for this.
How does Assisted Mechanical Ventilation Work?
Assisted mechanical ventilation provides support for the lungs through a tight mask fitted over the nose and/or mouth. This is attached via a tube to the ventilator which blows air into the lungs to help the patient breathe by supporting the muscles which make the lungs work. This is known as positive pressure ventilation. By assisting with breathing the aim is to reduce the levels of carbon dioxide and increase the oxygen levels in the blood.
Patients need at least 6 un-interrupted hours on the ventilator overnight to maximize the effectiveness of the treatment.
The mask can sometimes feel uncomfortable initially- the Home Ventilation Nurse will support the patient to get used to the sensation of the mask and air blowing on their face. As a Carer you will need to continue to support the patient with this.
Breathing can become less regular when people sleep, the ventilator helps to make sure patients take the right number of breaths per minute. In this way both the rate and depth of breathing will stay level even while they are asleep. Most people need to use the ventilator throughout the night however some people may require to use it during the day as well.
When the patient is initiated on the ventilator the Home Ventilation Nurse will assess the correct mask to use and adjust the settings on the machine- as a Carer you can be shown how to correctly fit the mask and start the ventilator in order to give support to the patient. It may take time to adjust to using the mask and ventilator however most people get used to it fairly quickly- if you have any questions or concerns, please discuss this with a member of the team.
This is a relatively simple treatment to use, and carers will be given support and advice to manage the treatment and patient’s condition as appropriate. Regular training sessions for Carers are available at the Home Ventilation Department at Castle Hill Hospital- please contact us if this is required.
Mask fitting
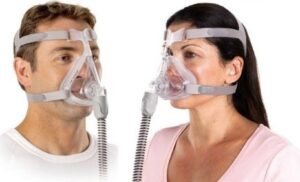
Mask fitting may feel strange for the patient at first but will become easier with practice. The mask does not need to be overtightened- loosening the mask may sometimes help to reduce leaks and discomfort. Support the patient with practicing putting on and removing the mask during the daytime may help with compliance.
Always fit the mask to the delve in the chin then place upwards on to the face. This prevents the mask from sitting too high on the nose which will cause leaks. Once the mask is in position on the patients face, hold it with one hand and slide the straps over their head with the other hand. Adjust the straps so that the mask fits snuggly against their face. Position the lower straps well down at the back of the neck, so that they pass below the ears. Try to adjust the straps evenly on both sides.
Once the ventilator is started, tighten the straps to make sure the mask fits without air leaking around it. You may need to readjust these straps once the patient is lying down.
The ventilator is designed to compensate for some leakage of air, so it is best to avoid over tightening the mask as this can cause skin damage to the face, as well as affecting the leak. There should be a slight movement of the mask on the face when the ventilator is in use- this is normal.
If oxygen is required while the patient is on the ventilator and adapter will be supplied. Ensure this is connected and the concentrator turned on when the patient is using the ventilator as instructed.
If the patient wakes in the night and feels uncomfortable with any aspect of the mask or ventilator, stop the ventilator and take the mask off for a few minutes. Help them to clear their nose if necessary and then put the mask back on and recommence treatment. Ensure they drink plenty of fluids during the daytime to prevent excessive mouth dryness while on the ventilator.
Trouble shooting problems
Common side effects people experience are: –
- Wind or a Distended Stomach- gulping air can cause this. Sleeping propped up may help. Peppermint tea/ water may relieve some of the discomfort. Avoid feeding the patient just before going on ventilation. If the problem persists inform the Home Ventilation Nurse who may be able to adjust the ventilator settings.
- Sores to the face and nose- this is caused by the mask being too tight. Loosen the mask and then reposition it. Mask fitting can take a lot of practice and patience to get it fitted properly. If problems persist inform the Home Ventilation Nurse as advice can be given regarding dressings and other masks are available.
- Sore Eyes- this is caused by air leaking from the mask and blowing into the eyes. Loosen the mask and reposition it. Do not continue with the air blowing into the eyes as this may cause significant, permanent damage to the corneas.
- Dry Mouth- The patient needs to drink plenty throughout the day to ensure they are hydrated and to avoid them becoming too dry overnight. Please discuss with the Home Ventilation Nurse if this is a problem as there are additional filters and humidifiers that may help.
- Nasal Irritation/ Congestion- Occasionally the treatment can cause irritation to the inside of the nose giving symptoms of a runny nose and sneezing or a feeling of being blocked and congestion. This may settle on its own, but if it doesn’t then nasal sprays may help- contact a pharmacist for further advice.
Ventilator Alarms: –
As we use a number of different ventilators we cannot list every different alarm. If you are unable to solve the problem from the following, please take a note of what the alarm says and contact the Home Ventilation Nurse.
- Circuit Disconnection- the ventilator has detected a large leak. Check the tubing is connected correctly and that there are no cracks or splits. Reposition the mask until the leak is eliminated -DO NOT over tighten the mask as this will make the leak worse.
- High Volume- again this can be due to a large mask leak- reposition the mask until the leak is eliminated. Alternatively check the tubing is not kinked or trapped.
- Internal battery in use – There has been loss of external power. Check if there has been a power cut or the electricity cable has fallen out of the back of the ventilator.
- External power failure – There has been a power cut, or the electricity cable has fallen out of the back of the machine. If there is a power cut contact your electric supplier who may be able to give an update as to when power will be reconnected.
- System Failure- In the event of an equipment failure please contact the Home Ventilation Office by telephone or email. In an emergency out of hours contact the Respiratory Support Unit on Ward 5, Hull Royal Infirmary. However, the majority of people are safe to manage overnight and contact the Home Ventilation Team on the next working day.
Care of equipment
Masks are very expensive; looking after the mask is the patients/ carers responsibility. If the mask and tubing is kept in optimal condition, it will last at least one year. One mask will be issued per year; if additional masks are required these can be purchased direct from the manufacturer. Please discuss with the Home Ventilation Nurse which mask you require.
Daily cleaning- each morning use a clean damp cloth to wipe around the mask to remove any oil or saliva build up. Leave the mask to air dry, ensure it is not in direct sunlight and do not place near a source of direct heat.
Weekly cleaning- Hand wash the mask and straps in a bowl of warm soapy water (use own brand washing up liquid). Rinse the soap from the mask and leave to air dry, ensure it is not in direct sunlight and do not place near a source of direct heat. Do not use a towel to dry as this will cause a buildup of static.
Tubing- this can be washed in warm soapy water, rinsed and hung vertically to air dry once a month.
DO NOT USE ANY GELS, WIPES OR ANY CHEMICALS ON THE MASK.
These can cause the mask to perish and cause damage affecting its use.
Cleaning- wipe the outside of the machine with a damp cloth. Ensure the machine is unplugged from the mains electric prior to cleaning. Do not immerse the machine in liquid. Most machines have a simple dust filter covering the air inlet- these should be changed every 3 to 6 months depending on the environment the ventilator is used in. The filter will be checked when your machine is serviced, but if it looks especially dirty please contact the Team for a replacement.
The ventilator has a green label on the side to say when its next service is due. Please inform the Team when this date is approaching so that a replacement ventilator can be left for collection or be exchanged at the next clinic appointment with the Specialist Nurse.
The ventilator requires mains electricity. Some models have an internal battery- to ensure this is fully charged the ventilator should be plugged into mains electric socket at all times. Ventilators with an internal battery are portable- please speak to one of the Home Ventilation Team regarding a portable manufacturer designed bag.
Clinic Appointments
Clinic appointments with the Home Ventilation Nursing Team will be arranged as required. The patient’s clinical condition and response to treatment requires monitoring while using non-invasive ventilation. By consenting to start treatment the patient has also agreeing to attend these appointments. Failure to monitor effectiveness of treatment may be detrimental and affect their health.
During the appointment the Nurse will check ventilator settings and filters, if a service is due the ventilator will be exchanged- please ensure all machines are brought to clinic. A Capillary Blood Gas sample may be taken to check the effectiveness of treatment and to identify if any adjustments to ventilator settings are required. An Oximeter for overnight monitoring at home may also be given- the Nurse will explain how to use this equipment; this needs to be returned the next morning for the team to download the results.
This appointment is a good opportunity for patients or carers to ask any questions or raise concerns about treatment with the Home Ventilation Nursing team.
If the patient is unable to attend clinic appointments, please contact the Home Ventilation Team as soon as possible so that we can rearrange this to a more convenient time.
Contact information & hours of service
The Home Ventilation Service operates from Monday to Friday 08.00 to 16.00. (excluding Bank Holidays).
For advice or information regarding your Home Ventilation service contact us on
Tel: 01482 624130 (24 hour answering machine)
email hyp-tr.HUTH.HMVS@nhs.net
If you require emergency advice out of working hours, please contact the Respiratory Support Unit at Hull Royal Infirmary- tel: 01482 875875.
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Respiratory Medicine on tel: 01482 624130.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

