- Reference Number: HEY1395/2023
- Departments: Paediatrics, Physiotherapy
- Last Updated: 30 September 2023
Introduction
This leaflet has been produced to give you general information. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and the healthcare team, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
What is a Patient-Initiated Follow-Up (PIFU) pathway?
A patient-initiated follow-up (PIFU) means that we will not routinely book you an appointment, instead we are putting you in control of making your own appointments at a time when you need them most, within a given timeframe.
How does PIFU work?
You will have been given this leaflet because your healthcare professional is happy that you do not need to see them again unless you have a problem. If you do have any problems, you can contact the Paediatric Therapy department on the given telephone number and they will arrange an appointment, either by telephone or face-to-face if it is needed. You will be told how long after your injury that you can contact the Paediatric Therapy department, on the PIFU pathway if you need to be seen.
When should I call for a PIFU?
You can call to make an appointment if you:
- are not improving to a level that was expected;
- have worsening symptoms relating to your injury/condition;
- have a “flare-up”.
Please note, you can only initiate a PIFU appointment for the specific injury/condition you were originally referred to the Paediatric Therapy service for.
When should I not use PIFU?
- If your concern is related to different injury/condition.
- If the specified time period has lapsed, please contact your GP.
- If you need urgent medical advice you should contact your GP or NHS111.
What if I don’t need a PIFU follow-up appointment?
You do not have to arrange an appointment if you feel it is not required. If you don’t contact us to book an appointment within the specified timeframe, the PIFU will expire and you will be discharged back to the care of your GP. We will not contact you to book a PIFU appointment – it must be initiated by you.
Booking a PIFU follow up appointment:
You or your parent/guardian can make an appointment to see us if you have any concerns related to your specific injury/condition |
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Paediatric Therapy Department on telephone: 01482-674539.
What is a mallet finger?
A mallet finger is where the tip of your finger becomes bent towards your palm and you are unable to straighten it, you may experience swelling and pain as a result of this.
Mallet finger is usually caused by an injury to the end of the finger which causes it to bend further than normal. This results in a tear of the tendon that would usually straighten the end of the finger. This is known as a soft tissue mallet injury.
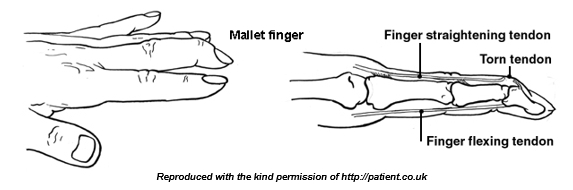
Sometimes a mallet finger is caused by a small piece of bone, where the tendon attaches, coming away from the bone with the tendon. This is known as a bony mallet injury. The effect of this will be the same, as the tendon is unable to straighten the end of the finger.
How should it be treated?
A splint will have been fitted to the tip of your finger which will keep the tip of your finger straight. This allows the tendon/bone to stay together and heal. This will take 8 weeks for a soft tissue mallet and 6 weeks for a bony mallet.
The splint should fit securely, not cause any soreness, and not become loose or fall off. The splint should be worn at all times, including when you are in bath/shower and when you are in bed, during this first period of continuous splinting. If you do not follow these instructions your ability to straighten the end of your finger may not return to normal.
To manage your pain, we advise that you regularly take simple pain relief, which can be bought over the counter. If you have allergies or conditions, which prevent the use of pain-relieving or anti-inflammatory medication, please seek advice from your doctor or a pharmacist.
Hygiene
The splinted finger must be kept clean and dry at all times. If the skin becomes wet inside the splint, it will become very sore. It is important to wash both your finger and the splint at least once a day, following these instructions:
- Keep your finger flat on the table, cut the strapping, and slide the splint off your finger.
- Keep the end joint straight at all times by keeping your finger flat on the table. Wash and dry your finger and the splint, keeping your finger supported on the table, using soap and water. You may find it easier if someone helps you to do this each day. Any movement of the end of the finger will delay healing and may even cause permanent damage.
- Slide the splint back over the fingertip, still keeping the finger straight.
- Replace the strapping – this should cover the middle of the splint but not the middle joint of the finger.
Exercises
Your splint should only restrict movement at the top joint of your finger, not the middle joint. It is important that you continue to move the middle joint of your injured finger and your other fingers fully to avoid stiffness. Do not remove the splint to do this. You should try to move the middle joint of your finger 10 times, 3-4 times per day, but do not remove the splint.
Is there anything I should avoid?
Do not:
- try bending the end of your finger to test it has healed;
- try to alter your splint yourself;
- remove the splint for anything other than to clean the finger and splint as described in the hygiene section;
- wear rings on the affected finger. If the finger is swollen it may affect your circulation and interfere with the healing process;
- participate in sport for at least 8 weeks
If the end joint bends during the continuous splinting period, it will slow the healing. You will need to re-start splinting again from the beginning.
What do I do at 6 or 8 weeks?
At the end of your 6 or 8 weeks continuous splinting you can remove your splint for light activities such as dressing and eating. You will still need to replace the splint for night time and heavy activities such as repeated or forceful gripping, for the next 4 weeks. Gradually wean yourself out of the splint slowly over these 4 weeks. The finger usually feels stiff at first.
The following exercises should be performed slowly and regularly every day after the splint has been removed. The purpose of these exercises is to help you regain full movement. Little and often (a few of each movement every hour) is better that doing lots of repetitions.
1. Finger/thumb extension
Straighten and stretch your fingers/thumb as straight wide as you can. Hold for 10-20 seconds.

2. Hook
Bend your fingers and knuckles to make a fist as tightly as you can. Hold for 10-20 seconds.
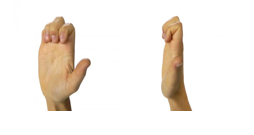
3. Full Fist
Bend your fingers and knuckles to make a fist as tightly as you can. Hold for 10-20 seconds.

If you lose any extension in the end joint after starting these exercises at 6 or 8 weeks, please stop doing the exercises and put your splint back on for continuous splinting and contact for a PIFU appointment.
What to expect?
Most mallet injuries heal well with splinting alone. The aim of splinting is to return the end joint to as near normal as possible. It is common for there to be a slight loss of full extension at the end joint of your finger at the completion of treatment.
It may take a few months for the swelling and tenderness to settle as well as the redness over the back of the finger. You may also find the skin of the finger may become more sensitive. You can massage the skin with a light moisturiser to help desensitise the skin.
Bony mallet injuries may leave a bump/deformity over the end joint of the finger. You may not regain full normal or pre-injury movement in the end joint of your finger. This generally doesn’t affect the overall function of the hand.
When should I call for a PIFU?
You should initiate a PIFU appointment if:
- pain and swelling is getting significantly worse;
- your splint does not fit well, it may be too tight or too loose, or prevent the middle joint of your finger from bending;
- you have any query regarding the length of time you need to stay in the splint or if the splint has come off before the allotted 6 or 8 weeks;
- you lose any extension in the end joint after starting the finger exercises at 6 or 8 weeks;
- 2 weeks after starting the exercises and weaning from the splint you are struggling to make a fist, or get your fingertip to your palm.
Or after 12 weeks, you are struggling to return to your usual work or hobbies.
If we do not hear from you 3 months following your injury date we will assume that you no longer require any further intervention and will be discharged from the PIFU pathway. If you have further problems with your hand after this date please contact your GP practice
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Paediatric Therapy Department on telephone: 01482 674539.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats your child, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to your child. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your child’s condition, the alternatives available for your child, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about your child
We collect and use your child’s information to provide your child with care and treatment. As part of your child’s care, information about your child will be shared between members of a healthcare team, some of whom you may not meet. Your child’s information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide your child with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your child’s doctor, or the person caring for your child.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about your child. For further information visit the following page: Confidential Information about You.
If you need information about your child’s (or a child you care for) health and wellbeing and their care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

