- Reference Number: HEY841/2025
- Departments: Major Trauma
- Last Updated: 31 August 2025
Hull Royal Infirmary – Major Trauma Centre
Information for patients and relatives
This booklet offers information to you and your carers about being in the Major Trauma Centre (MTC) at Hull Royal Infirmary, what has happened, what will happen, and how we can help you with your journey to recovery.
This booklet will provide you with all the information necessary for you, or your relatives during the stay. It should help keep all the useful information in one place.
If you require further information on topics that are not covered in this booklet, please speak to a member of staff in the department of your inpatient stay.
What is a Major Trauma?
Major trauma is a term used to describe any physical injury which can have potential serious complications. A typical example of this term would be an individual involved in a road traffic collision (RTC) with complex injuries and needs; a fall from a significant height or an assault causing serious injuries.
Due to the variable nature of this term, major trauma can be further categorised to describe what type of injury you or your relative has suffered, such as:
Blunt force trauma – a non-penetrating external or internal injury caused by blunt force
Penetrating trauma – an injury that penetrates through the skin to a space or organ within the body
Orthopaedic trauma – injuries involving the musculoskeletal system
Complex trauma – multiple injuries requiring multiple speciality team involvement
Burn injuries – moderate to severe burns covering more than 20% of a total body surface area
What is a Major Trauma Centre?
Although all hospitals can provide a range of treatments and cares, it is of utmost importance to provide major trauma patients with specialised care 24 hours a day. These hospitals are known as Major Trauma Centres (MTCs) and can provide the necessary multi-speciality care required for individuals.
Within an MTC, medical interventions can be found from specialities such as Surgery, Vascular Surgery, Plastic Surgery, Interventional Radiology and Rehabilitation Medicine.
Across England there are 8 Adult Major Trauma Centres, of which Hull Royal Infirmary is one. There are a further 12 Adult and Paediatric Centres, 4 Paediatric Centres and 2 Collaborative Centres.
Combined, these form a Major Trauma Network. Our network is known as the North Yorkshire and Humberside Operational Delivery Network and comprises of:
Hull Royal Infirmary
Diana Princess of Wales Hospital (DPOW) — Grimsby
Scunthorpe General Hospital
York Teaching Hospital
Scarborough Hospital
Our Major Trauma Centre, Trauma Unit and Network
Network of Major Trauma Units and Major Trauma Units
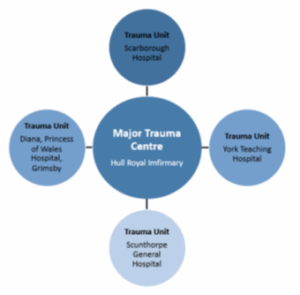
Why have I been admitted to Hull Royal Infirmary?
Each Major Trauma Centre and Trauma Unit work very closely with their pre-hospital care teams. Within our network, we engage with the following;
British Association for Immediate Care (BASICS)
East Midlands Ambulance Service
HM Coastguard Search and Rescue
Lincolnshire and Nottingham Air Ambulance
The Air Ambulance Service
Yorkshire Air Ambulance
Yorkshire Ambulance Service
On attending an incident, the pre-hospital teams conduct a multifactorial assessment which evaluates the current and potential risks to the patient. The assessment includes identifying immediate issues, such as obvious injuries that need instant attention. The crew will then take clinical observations, consisting of heart rate and rhythm, blood pressure, oxygen saturations and conscious level. If the crew are concerned with any of these measures, or the patient fulfils specific criteria set by NHS England, the crew will Pre-Alert the Major Trauma Centre within that region.
You may find that you/your relative was taken to a Trauma Unit Hospital before arriving at Hull Royal Infirmary. Depending on the severity of the injuries sustained, the ultimate aim may be to transport the patient to the Major Trauma Centre as quickly and as safely as possible. However, if the crew cannot make this journey within 60 minutes and the patient shows signs that life-threatening treatment is required to make the journey, then the patient is taken to the nearest Trauma Unit to stabilise them before safely continuing the journey.
What happens on my arrival at Hull Royal Infirmary?
The Pre-Hospital Team will alert the Emergency Department staff that a patient is on their way who fulfils criteria set on the Major Trauma Triage Tool.
Once this alert is received in the Emergency Department, a Trauma Call is activated to the Trauma Team within the hospital. The Trauma Team consist of;
Anaesthetist and Airways Assistant
Emergency Department Consultant
Emergency Department Senior Doctor
Emergency Department Nurse
General Surgeon
Major Trauma Nurse Specialist
Orthopaedic Surgeon
Radiologist
There are occasions whereby more than one doctor from each speciality attend the call; this is perfectly normal and is controlled by the team leader.
The aim of the Trauma team activation is that all main specialities are present for the arrival, so that we can provide the patient with the best care and treatment as quickly as possible.
The immediate investigations and treatment the patient receives will depend on the injuries and their severity. Each patient will receive what we call a Primary and Secondary Survey. These are explained further on in this booklet.
What happens next?
This part really depends on what injuries the patient has sustained and to what extent, although ultimately all options have the same goal……
From admission to discharge, we aim to deliver the best care and treatment in the most timely and effective manner.
It is quite rare that an individual who triggers a Trauma Call is discharged home from the Emergency Department, but this does happen from time to time. If the injuries require further treatment or you/your relative’s condition is for further observation, then there are three main areas from the Emergency Department; Theatre, the Intensive Care Unit or the Major Trauma Ward. The Emergency Department staff will be able to give the you/your relatives an idea of where the admission is likely to be, or where the patient will go to after theatre.
It is sometimes necessary that once a patient has been assessed by the Trauma Team, they are required to transfer to Castle Hill Hospital for specialist Cardiothoracic treatment and surgery. Castle Hill Hospital is our second acute centre within the Hull University Hospitals NHS Trust, based in Cottingham.
All relevant ward contact numbers and visiting times have been provided for you later in this booklet.
Throughout the in-patient stay, overall medical care is provided by the Consultant-Led Speciality teams, and all patients are monitored by both our Major Trauma Consultant and four Major Trauma Coordinators. The Consultant and Coordinators will liaise with the appropriate wards and specialities to help support the recovery of you/your relative.
Your Major Trauma Team
In addition to the specialist team you have been admitted under, and the ward nursing and therapist team, you should be seen every weekday by the Major Trauma Consultant. A number of Consultants undertake this role from a variety of specialities to ensure your care is well managed and when senior input is required across a number of specialities they are able to facilitate this.
We have a team of specialist nurses, Major Trauma Nurse Specialist, who you will meet during your admission. They are often part of the ‘Trauma Team’ who managed your care in the Emergency Department. They work alongside the Major Trauma Consultant to ensure the various specialities involved in your care connect smoothly, plans are clear and you are kept informed about any developments in your care, this team of nurses follows you throughout your stay at Hull Royal Infirmary, whichever in-patient department you are in.
Enduring a Major Trauma can have a significant impact on your mental health. Because of this, within our team, we have a Major Trauma Clinical Psychologist. Once referred to the Psychology service our Psychologist will aim to see you during your inpatient stay and/or will provide information regarding where to seek help should you require it after your discharge.
A Chaplaincy Service is available 24 hours a day. If you feel that as a patient or a relative you would like to see a chaplain, please inform the staff who can con- tact the team on your behalf. Alternatively, you can ring the team within office hours on tel: 01482 675966, or via switchboard tel: 01482 875875 out of hours.
A multi faith room is situated on the first floor at Hull Royal Infirmary and near to Ward 11 at Castle Hill Hospital should you wish to visit.
Whatever your religion, we can help find you a faith-specific representative to talk to.
The Multi-Disciplinary Team Involvement
Alongside the Medical and Nursing teams, an array of professionals work together in order to offer a thorough and appropriate care management pathway. The following list highlights just some of the professionals who work together in providing a Multi-Disciplinary Team;
Acute Pain Services
Clinical Pharmacists
Clinical Psychology and Mental Health
Dieticians and Speech and Language Therapists
Head Injury Specialist Nurse (Headway)
Major Trauma Coordinators
Occupational Therapists
Physiotherapists
Rehabilitation Coordinators
Social Workers, Specialist Nursing and Therapy groups
Throughout the hospital stay, patients may be referred to one, or many of our specialist professionals within the Multi-Disciplinary Team. As a service we do not only look at the current medical circumstances of an individual, but that of potential discharge problems, and aim to provide both the patients and their relatives with the most appropriate support for going home.
If you feel that you/your relative needs any support or foresee potential issues on discharge, please inform the staff as soon as possible.
What happens next?
This part really depends on what injuries the patient has sustained and to what extent, although ultimately all options have the same goal……
From admission to discharge, we aim to deliver the best care and treatment in the most timely and effective manner.
It is quite rare that an individual who triggers a Hospital Trauma Call is discharged home from the Emergency Department, but this does happen from time to time. If the injuries require further treatment or you or your relative’s condition is for further observation, then there are three main areas from the Emergency Department; Theatre, the Intensive Care Unit or the Major Trauma Ward. The Emergency Department staff will be able to give the you or your relatives an idea of where the admission is likely to be, or where the patient will go to after theatre.
It is sometimes necessary that once a patient has been assessed by the Trauma Team, they are required to transfer to Castle Hill Hospital for specialist Cardiothoracic treatment and surgery. Castle Hill Hospital is our second acute centre within the Hull University Teaching Hospitals NHS Trust, some six miles East.
Throughout the in-patient stay, overall medical care is provided by the Consultant-Led Speciality teams, but all patients are monitored by our Major Trauma Consultants and Major Trauma Coordinators. The consultant and coordinators will liaise with the appropriate wards and specialities to help support the recovery of you or your relative.
The Primary and Secondary Survey
The Primary Survey is a quick and efficient assessment completed by senior medical staff, aiming to identify any injuries that are life-threatening or of concern. Anything identified at this stage is immediately treated. Examples of this may be that a chest drain is inserted to allow adequate breathing, a blood transfusion may be swiftly administered in order to maintain an adequate blood pressure, or a breathing tube may be placed if there is a low conscious level.
Within this period other members of the team are jointly working alongside each other to gain Intravenous access (a cannula into the vein) to administer necessary fluid, blood or medication. Blood samples will be sent and arrangements for further investigations are commenced here.
Although the Radiology team are aware of the patient’s imminent arrival, Computerised Tomography (CT) Scans, X-rays and Ultrasound Scans are examinations which will be requested at this stage. If appropriate, and as soon as the patient is stable enough to transfer to the CT scanner, the team escort the patient for their necessary scan(s). Specialist Radiologists begin to view the images to identify any injuries sustained and their severity, enabling the team to plan ahead.
The Secondary Survey takes place once all immediate risks are being man- aged. This assessment checks all of your systems from head-to-toe in order to identify anything that could have been missed, or that was not deemed life- threatening during the Primary Survey. An example is to X-ray a fractured limb and place this within a cast, or checking if there is sensory loss to limbs should there be a neck or back injury. If required, further specialist teams are called at this point for their assessment. If admission is necessary, a speciality team is allocated to you in the Emergency Department.
Car Parking
Our main Hull Royal Infirmary car park on Argyle Street, and all of our patient and visitor car parks at Castle Hill Hospital, now use Automatic Number Plate Recognition (ANPR).
A camera will read your number plate as you drive into our car park.
You will need to “pay on exit” before returning to your car.
When you reach the exit, the barrier will lift as long as you have paid.
Some of our smaller car parks at Hull Royal Infirmary are still pay-and-display, please check the signs in the car parks.
Charges:
£2.00 for up to 1 hour
£3.00 for 1 to 2 hours
£5.00 for 2 to 24 hours
£10.00 for 1 week
£15.00 for 2 weeks
£20.00 for a month
If you are going to be attending hospital regularly for a short period of time, you can save money by purchasing an unlimited parking permit. You must ask for a form from the ward or department you are visiting, then take it to the Security Office at either of our hospitals.
If you are travelling from west of the A63 is the Priory Park, Park and Ride facility in Hessle. Situated a short drive from the hospital, you can park and travel to Hull Royal Infirmary for a small charge.
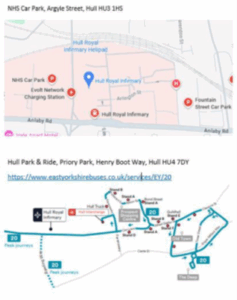
Another option if you are travelling from west of the A63 is the Priory Park, Park and Ride facility in Hessle. Situated a short drive from the hospital, you can park and travel to Hull Royal Infirmary for a small charge.
Travelling to Hull Royal Infirmary
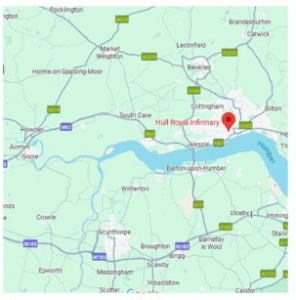
Contact Numbers and Visiting Times
Below are a few useful numbers that will take you directly where you need to be;
Hull Royal Infirmary and Castle Hill Hospital Switchboard tel: 01482 875875
Major Trauma Ward (based on Ward 40) tel: 01482 675041 or tel: 01482 675040
Intensive Care 1 at Hull Royal Infirmary tel: 01482 311727 or tel: 01482 311737
Intensive Care 2 at Hull Royal Infirmary tel: 01482 311732 or tel: 01482 311733
Intensive Care 1 at Castle Hill Hospital tel: 01482 461511 or tel: 01482 461514
Intensive Care 2 at Castle Hill Hospital tel: 01482 623179 or tel: 01482 622670
Patient Advice Liaison Service (PALS) tel: 01482 623065
Visiting Times of wards;
Major Trauma Ward and Ward 38 – 11:00 – 20:00
Intensive Care Units 1 and 2 at Hull Royal Infirmary – 12:00 – 22:00 (Please note that visitors will have to wait in the waiting room during the nurses handover period)
Intensive Care Units 1 and 2 at Castle Hill Hospital—12:00—22:00 (Please note that visitors will have to wait in the waiting room during the nurses handover period)
We advise that you call the ward prior to visiting to confirm times, as these are subject to change.
Please note, due to the distance some relatives may have to travel, it may be possible to extend your visiting hours. Please ring and ask the Nurse in Charge before you set off.
Food and Amenities
Food and drink is available from the café & restaurant situated on the ground and first floors of the Tower Block or the café within Women and Children’s Hospital.
Their opening times are below:
Costa Coffee (ground floor)
Monday to Friday 07:30 – 20:00
Saturday & Sunday 07:30 – 17:30 Both Hot and cold food
Nourish Restaurant (first floor)
Monday to Friday 07:30 – 19:30
Saturday & Sunday 07:30 – 19:30 Both hot and cold food
The Orchard Café (Women and Children’s Building)
Monday to Sunday – 08:30 – 16:00
Both hot and cold food
Vending machines are available in the Nourish Restaurant that can be used 24 hours a day serving both hot and cold food.
Pharmacy and Retail
WH Smith’s shop is situated on the ground floor of the Main Building and opens at the following times:
Monday to Friday – 07:00 – 19:30
Saturday & Sunday 09:00 – 19:00
Lloyds Pharmacy is also situated on the ground floor within the entrance to the reception area:
Monday to Friday – 08:30 – 18:00
Saturday 10:00 – 14:00
Sunday Closed
Services you may be able to access
Citizens Advice Bureau
We are able to ask a member of staff from the Citizens Advice Bureau to come and see you in hospital to assist with concerns you may have regarding bene- fits you may claim and any entitlements you may have if you are unable to work due to your injury. Please let us know if you would like to be referred.
Stewarts Law
Stewarts legal team work with the Trust and provide a free service to patients who have been on the Intensive Care Unit or who have had a Major Trauma. They can help with a variety of issues including:
Welfare benefits
Housing
Financial issues (including if you are worried about debts accruing during your stay).
Insurance and employment issues
Powers of attorney
Post discharge care
If you would like to be referred to this service please let the ward staff know.
There are a wide variety of organisations, Charities and support networks potentially available to you. We have a noticeboard on ward 38 with more details or please ask a member of staff.
Rehabilitation and preparing for discharge
Rehabilitation is a key aspect to recovery for patients who have suffered Major Trauma and involvement from different professionals within the Major Trauma team will support patients during their hospital stay. The team meets on a daily basis Monday to Friday to discuss patients’ rehabilitation needs and plans necessary to help recovery.
Where possible patients will be discharged straight home however this may not always be possible as some patients may need more time to recover from their injuries. If this is the case the team will talk to the patient about further rehabilitation and where this is likely to be based on where they live and what their needs are.
Rehabilitation will be planned with patients by staff involved in their care and will look at medical, physical, sensory and psychological needs. The team will complete their assessments and base treatment plans on the specific needs of each patient whilst in hospital as well as what they may require to support with planning for ongoing rehabilitation or discharge home (such as further inpatient or community rehabilitation, provision of equipment, or a package of care to support at home).
If a patient’s local hospital is not Hull Royal Infirmary and further rehabilitation is required, support or equipment at home is needed or they have ongoing medical needs they may be transferred back to a more local hospital for this to be arranged. This is called repatriation. The teams in the local hospital will continue to help recovery and make plans for ongoing rehabilitation or discharge.
Emotional Wellbeing
An admission to the Major Trauma service can be a very distressing and stressful experience. Patients have often been through highly traumatic accidents and incidents. Patients may have also experienced significant or life changing injuries and may require extensive treatment or medical interventions that may be difficult to cope with.
Patients can experience a wide range of emotional and psychological difficulties, both during their admission and following discharge home. These reactions can sometimes be difficult to cope with, as they may include emotions, thoughts and feelings that we are not used to experiencing.
Some people experience little or no distress and others describe ‘positive psychological reactions’ – there is no right or wrong way to feel following a traumatic event.
You may feel you have encountered many of the following difficulties, or that very few apply to you. Whatever your experience, we would encourage you to discuss any psychological difficulties or concerns that you have with our team, as your psychological wellbeing is a very important aspect of your treatment and recovery.
Common difficulties reported by patients include;
Low mood, feeling upset and tearful
Anxiety, worry, fear and panic
Feeling scared about the severity of your injuries, particularly if they were life threatening
Shock and difficulties coming to terms with or adjusting to your situation Feeling irritable, frustrated or short tempered. Sleep difficulties including disrupted sleep, vivid dreams and nightmares
Experiencing distressing thoughts, images, flashbacks or memories Feelings of guilt or concerns about the impact on others close to you Worry about the future and about your recovery
Difficulties associated with fatigue
Memory difficulties, feeling forgetful, periods of confusion and disorientation
Feeling isolated, unable to express how you feel or the sense that others do not understand your experience
Feeling overwhelmed
This list is not exhaustive, but may capture some of your difficulties. Please speak to a member of our team if you feel that you are experiencing any psychological and/or emotional difficulties which you feel you need support with.
Whilst on the ward, you can be referred to the Major Trauma Clinical Psychologist, who will be able to offer you support during your admission and who can help you to access further psychological support once you are home. Please also speak with us if you feel that your relatives or friends require support in relation to your situation- we can also signpost them to appropriate services that allow them to access their own support.
If these difficulties become more apparent to you following your discharge home, please seek support from your GP. Difficulties can occur immediately or may start after a delay of some days or weeks. For some people, an emotional reaction might last for a short period of time, perhaps only hours, whereas for others this may go on for several weeks. If you feel your symptoms are not improving or are worsening over time, if you find them over- whelming or if you are struggling to cope, please discuss this further with our staff or with your GP following discharge.
Accommodation
It may be necessary for relatives to stay close to the hospital and we recognise that some relatives may have travelled a long distance to the hospital.
Below is a list of some local hotels and Bed and Breakfasts either within walking distance or a short car drive from the hospital:
Please note, in providing these details the trust is not making a recommendation and that other venues are available
Holiday Inn – tel: 0871 942 9043 /
Holiday inn Express – tel: 01482 485700 / www.ihg.com
Ibis Hotel – tel: 01482 387500 / www.ibis.com
Kingston Theatre Hotel – tel: 01482 225828 / www.kingstontheatrehotel.com Travelodge Hull Central – tel: 0203 195 4924 / www.travelodge.co.uk
Premier Inn – tel: 0871 527 8534 / www.premierinn.com
Should you need to stay nearby to Castle Hill Hospital, the following hotels are a short drive away:
Inn Keeper’s Lodge – tel: 01482 651518 / www.innkeeperslodge.com
Willerby Mecure Grange Park Hotel – tel: 0844 815 9037 / www.mercurehull.co.uk
Please Note, limited accommodation is available at Hull Royal Infirmary in exceptional circumstances.
Patient Advice and Liaison Service (PALS) and Complaints
Sometimes things do not go just as you would like them to. In the first instance, we would ask you to speak to the staff in the ward or department.
Many problems can be resolved quickly by talking to the staff who are involved in your care. Misunderstandings can happen and can often be resolved quickly. Speak to the nursing staff looking after you or your relative or ask to speak with the nurse in charge.
If you feel that you are not able to speak directly to staff caring for you, the Patient Advice and Liaison team can help you. The Patient Advice and Liaison Service (PALS) at Hull Royal Infirmary provides support and information to patients, their families, and carers.
They can help with concerns, complaints, and general queries about hospital services.
You can contact PALS by phone at tel: 01482 623065, by email at hyp-tr.pals.mailbox@nhs.net , or by visiting them at Alderson House, Hull Royal Infirmary, Anlaby Road, Hull, HU3 2JZ
This patient information leaflet has been created for use at Hull University Teaching Hospital – Major Trauma Centre only.
Hull Royal Infirmary Major Trauma Centre Booklet
Created by Leah Dobson – Major Trauma Coordinator
Arranged & Edited by Alex Bampton – Admin Apprentice and the Major Trauma Team

General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.



