- Reference Number: HEY1286/2022
- Departments: Orthopaedics, Physiotherapy
- Last Updated: 30 September 2022
Introduction
This leaflet has been produced to give you general information. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and the healthcare team but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
What is a finger and thumb interphalangeal (IP) joint dislocation or thumb metacarpal (MCP) joint dislocation?
The finger and thumb interphalangeal (IP) joints are the small joints of the fingers and thumb. They are the joints between the finger bones (see below) and there are two in each finger. There is one interphalangeal joint in the thumb (IPjt). The thumb metacarpal joint (1st MCPjt) is the joint between the thumb bone and the hand bone.
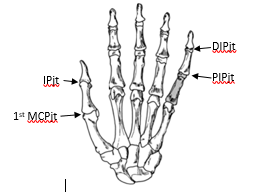
A dislocation of these joints is when the bones of the joint come abnormally away from each other. If the bones are only partly separated this is called a subluxation. It is quite common for there also to be a small break/fracture of the joint bones this is an avulsion fracture.
How should it be treated?
Any dislocated or subluxed joint needs to be put back in place as soon as possible (reduced). This is sometimes done immediately if there is someone present who can perform the procedure. More frequently it will be done in the local Accident and Emergency department.
If the joint is reduced quickly and the joint is stable, good recovery can be expected. The finger may be temporarily strapped to the adjacent finger to provide support but should not prevent movement. The tape should be applied in thin strips above and below the affected joint. This tape should be removed, the hand washed and reapplied on a daily basis. Tape should be discarded completely at 2 weeks.
What should I do in the first few days?
The affected joint will be swollen and stiff. It is important to gently and regularly move the joint. Complete rest is not advisable. It is important that you try to use your hand normally when doing everyday tasks such as washing, dressing and eating.
Exercising the finger or thumb early is very important to prevent stiffness. The following exercises should each be repeated 10 times and completed every 2-3 hours. Support your elbow on the table with your wrist straight.
-
- Finger/thumb extension 2. Hook
Straighten and stretch your fingers/thumb Bend your fingers/thumb at
as straight/wide as you can. the small joints. Hold 10 to 20
Hold 10 to 20 seconds seconds


3. Full Fist 4. Opposition
Bend your fingers and knuckles Take the tip of your thumb across
to make a fist as tightly as you can. to the tip of your little finger. Then
Hold for 10 to 20 seconds. down the little finger. Hold the stretch for 10 to 20 seconds.


Images taken by Medical Photographer, Plastic Surgery, NHS Humber Health Partnership
Swelling
Swelling is a normal reaction following joint dislocation and can take several months to settle fully. It is important to minimise this as much as possible by doing the following:
- Elevate the hand, especially at night on pillows.
- Ice – massage with an ice cube. Remembering to keep it moving.
- Massage along the finger or thumb towards the wrist.
- Complete the exercises above
When can I drive again?
You may not be insured to drive whilst your fingers have strapping in place. It is always good to check with your insurance company.
It may be safe to return to driving when:
- You are no longer using the strapping
- You can comfortably grip the steering wheel, move the gear stick, pull up the hand brake and activate the indicators
- You can perform an emergency stop
What about work and sport?
If you have a job with light or clerical duties, you can work as soon as you feel comfortable.
Heavy manual work is best avoided until 6 weeks after your injury.
Full contact sport should also be avoided for at least 6 weeks
Possible complications and when to initiate PIFU?
Joint stiffness and a flexion contracture (the joint remaining in a bent position) are the most common complications. These can be avoided by following the above information regarding minimising swelling and encouraging movement. However, on occasion this will still develop.
Please initiate a Patient Initiated Follow UP (PIFU) appointment if
- You are struggling to fully straighten your finger or thumb at 2 weeks following your injury or you feel it is getting worse
- You are struggling to make a full fist or reach the base of your little finger with your thumb tip at 3 weeks following your injury
- You feel your movement or function is worsening
- Your pain or swelling worsens
Details of how to book a PIFU appointment can be found in the PIFU leaflet which you will have received alongside this leaflet. If we do not hear from you 3 months following your surgery date, we will assume that you no longer require any further intervention and will be discharged from the PIFU pathway. If you have further problems with your finger after this date, please contact your GP practice
Should you require further advice on the issues contained in this leaflet or wish to initiate a PIFU appointment, please do not hesitate to contact the Physiotherapy Department on telephone: 01482 674880.
Your feedback matters to us…
To ensure we deliver a safe and quality service and to help us understand the experience you have of the care you receive from our staff we would value your thoughts about the service you received.
You may be contacted as part of our quality assurance programme which is where we visit our teams and staff and talk to them about the care they provide to our patients or at any time during or after you have needed our services.
To collect this feedback, we would contact you using the registered telephone number we hold in your care record. This feedback will be strictly anonymous and whilst we will share the feedback as part of the process, we will not share any details which may identify you.
We will never ask you any personal questions about your health during these telephone calls.
If you do not wish to speak to us, please say this when we call, we do not want you to feel pressured.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

