- Reference Number: HEY200/2024
- Departments: Renal Service
- Last Updated: 30 September 2024
Introduction
This leaflet has been produced to give you general information about your procedure. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and the surgeon, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
What is a fistula?
A fistula is formed when a surgeon joins an artery and vein together, just under the skin. It is most frequently created in your forearm. No foreign body or plastic material is used to create most fistulas. The fistula is made using your own blood vessels, reducing the infection risks compared to having any artificial material in the body like a dialysis line or catheter.
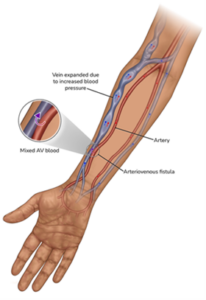
Image from Kidney Care UK.
Why do I need a fistula?
When a person requires haemodialysis treatment a reliable route to your blood supply is essential. Having a good fistula will enable the nursing staff on the Haemodialysis Unit to place two needles into the fistula and attach you to the haemodialysis machine. Once a fistula has been created it will take 6 to 12 weeks for it to mature. A mature fistula will allow safe, reliable and repeated access to your circulation for haemodialysis.
Can there be any complications or risks?
Most people have no major complications with this operation. Complications and risks that may affect some people are:
- Mild or moderate bleeding from the wound site after the operation
- Infection of the skin around the surgical wound
- Sensation problems in the hand of the fistula, which often improves with time
- Coolness in the hand of the arm where the fistula is made; so called steal syndrome
- Fistula failure-up to 1 in 5 fistulas may clot or fail to mature (develop) and a further procedure may then be needed to try and help the fistula mature require a new fistula to be made
If you have any concerns or questions regarding the risks or complications, please speak to the surgeon who will be doing your operation.
How do I prepare for the fistula?
Please read this information leaflet. Share the information it contains with your partner and family (if you wish) so that they can be of help and support. There may be information they need to know, especially if they are taking care of you following this procedure.
You will be seen by the surgeon and possibly the access nurse in a clinic or on the ward where:
- Examination of your arms will take place to assess the quality of your veins; you will also likely have an ultrasound scan of the arm.
- A decision is made where your fistula will likely be created. Where possible the surgeon will try and avoid putting the fistula in the arm you use the most. After the operation, your arm may benefit from being rested a little over the first few days and you may feel restricted in what you can do.
- Ideally you will be able to get back to all normal activities quickly, you should also try to exercise the hand on the side of the fistula with squeezing a ball or similar to help promote blood flow
- You will be given a date and time for the operation or placed on a waiting list. Most operations are carried out as a day case and are performed under a local anaesthetic (you will be awake throughout the operation). The local anaesthetic will numb the area that will be operated on.
IT IS VERY IMPORTANT that once the surgeon says which arm he will be operating on you do not let anybody take blood or put a drip in that arm. The back of your hand or other arm should be used.
On the day of the initial assessment, you may bring someone with you to the clinic. However, for the day of surgery you should attend on your own. You will be advised where your operation will take place.
If you are taking warfarin or any other blood thinning medication your surgeon will advise you whether to stop this medication or not before your operation.
What will happen?
You will be asked to sign a consent form for the operation you are having and you should only sign this when you are sure you have:
- Understood the reason for the fistula
- Understood how the operation will be performed
- Understood the risks that could be involved
If you are unclear about anything please ask the doctor or nurse looking after you.
- Once in the operating theatre you will be given a local anaesthetic. This will numb the area the surgeon will be operating on. You may feel a stinging sensation when the local anaesthetic is put in. During the operation you might feel movement and pressure as the surgeon is working but you should not feel pain. If you feel any pain please let the surgeon know and they will give you some more local anaesthetic.
- Once the surgeon has joined the artery and vein together they will use dissolvable stitches to close the skin to avoid any discomfort of having stitches removed.
What happens afterwards?
- Immediately after the surgery your arm will be elevated on a pillow and will be wrapped in a blanket to keep it warm.
- If you experience any pain in your arm after the operation you will be given simple pain relief medication such as paracetamol.
- Most patients will be discharged the same day.
- You will be taught how to feel your fistula for a “thrill” (a light buzzing) to check that it is working. You should check this daily.
- It will take between 6 to 12 weeks for your fistula to be ready to mature.
- Sometimes the first attempt at creating a fistula may fail. If this happens you will be seen again by the surgeon. One in four fistulas will not develop at the first attempt.
- You will be given a going home information leaflet with instructions on how to look after and care for your fistula.
- If you do not have a clinic appointment with the renal doctors or are not on haemodialysis the access nurse will make an appointment for you to make sure your fistula is developing approximately 4 to 6 weeks after your operation.
PLEASE CONTACT THE ACCESS NURSE PRACTITIONER ON tel: 01482 608709 IF YOU HAVE ANY QUESTIONS
IF YOU CAN NO LONGER FEEL THE BUZZING OF YOUR FISTULA PLEASE RING THE RENAL WARD ON tel: 01482 674980 IMMEDIATELY FOR ADVICE
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

