- Reference Number: HEY924/2025
- Departments: Emergency Department, Paediatrics
- Last Updated: 31 May 2025
Introduction
This leaflet has been produced to give you general information about your child’s condition. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and your child’s doctor, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for your child.
Fever in Children
Fever (high temperature, usually above 38C) is the body’s natural response to infection. Your child has been examined and the doctor has decided that your child does not need to stay in hospital. It is not always necessary to reduce a fever. Treatment with paracetamol or ibuprofen can make your child feel better if they are distressed, but will not treat the cause of the fever or prevent complications such as a febrile convulsion. The height of a temperature does not help to decide how unwell a child is (except in babies under 6 months old). Most feverish children do not need antibiotics.
Care at Home
- Offer your child regular fluids. If you are breastfeeding your child, continue to do so.
- If your child has a rash do the ‘tumbler test’ – see below.
- Check your child during the night.
- Keep your child away from nursery or school while their fever persists.
- Do not sponge your child with water. This does not help to reduce fever.
- Dress your child normally. There is no need to over- or under-dress them.
- Consider using paracetamol or ibuprofen if your child appears to be distressed by the fever.
The Tumbler Test or Glass Test
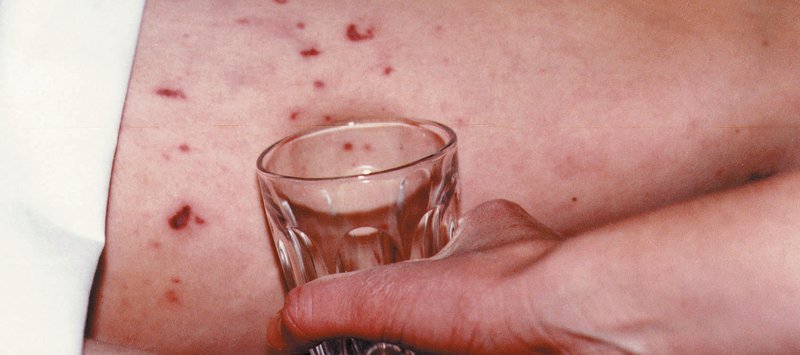
Photo courtesy of the Meningitis Research Foundation
- Press the side of a clear glass firmly against the skin over the rash.
- Fever with spots/rash that do not fade under pressure could be a medical emergency. Ring 999 immediately.
- If your child is ill and getting worse, get medical help immediately. Do not wait for a rash to appear.
- On dark skin, the spots/rash can be more difficult to see so look for rashes on paler areas such as palms of the hands, soles of the feet or the tummy.
Contact your GP or call NHS 111 if:
- Your child’s health gets worse or if you are worried.
- Your child is not drinking.
- Your child seems dehydrated, for example dry mouth, sunken eyes, no tears or a sunken soft spot on a baby’s head.
Call 999 or attend the Emergency Department if:
- Your child becomes pale and floppy.
- Your child becomes difficult to wake.
- Your child is finding it hard to breathe.
- Your child has a fit.
- Your child develops a rash that does not disappear with pressure (the tumbler test).
Should you require further advice on the issues contained in this leaflet, please call NHS 111
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats your child, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to your child. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your child’s condition, the alternatives available for your child, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about your child
We collect and use your child’s information to provide your child with care and treatment. As part of your child’s care, information about your child will be shared between members of a healthcare team, some of whom you may not meet. Your child’s information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide your child with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your child’s doctor, or the person caring for your child.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about your child. For further information visit the following page: Confidential Information about You.
If you need information about your child’s (or a child you care for) health and wellbeing and their care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

