- Reference Number: HEY1355/2025
- Departments: Physiotherapy, Therapies
- Last Updated: 30 September 2025
Introduction
This leaflet has been produced to give you general information about your procedure. Most of your questions should have been answered by this leaflet. It is not intended to replace the discussion between you and your doctor/hand therapist but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team who has been caring for you.
What is the Central Slip?
The central slip makes up part of the extensor tendons of the fingers. The extensor tendons connect the muscles to the bone and are responsible for straightening your fingers. The central slip works on straightening the middle joint of your finger. Injury to the central slip usually occurs from the finger being traumatically forced into a bend, e.g. being hit by a ball, or if the joint dislocates.
Splint and Elevation
A thermoplastic splint will be made and fitted to you to keep the middle joint of your finger straight. This allows the tendon to heal in a good position. If the splint doesn’t fit/becomes loose, contact your hand therapist as soon as possible. It is vital that you DO NOT remove the splint until advised to do so by your doctor or hand therapist. Swelling is a normal reaction to injury; however, it is important to limit this as much as possible:
- Keep your hand elevated when wearing your splint
- Elevate your hand on pillows at night
- If your hand remains swollen continue the elevation until it settles
Exercise
Exercise is important to allow your tendon to heal and will reduce stiffness and swelling in your finger. The hand therapist will demonstrate the exercises which you should continue to do regularly at home. Keep your splint on during both exercises.
ACTIVE DIP JOINT FLEXION
Use your unaffected hand to firmly hold the splint between thumb and fingers, bend the tip joint as far as able. Hold 3 seconds before straightening it.
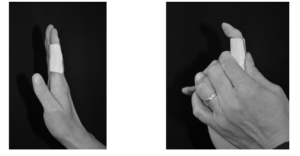
ACTIVE MCPJOINT FLEXION AND EXTENSION
Bend your fingers from the knuckles, making sure that you keep your fingers straight. Hold for 5 seconds

Repeat the exercises ________ times every ______ hours
General Advice
- You can use your hand for daily activities with the splint remaining in place – however, you should avoid heavy gripping or lifting until advised by your hand therapist.
- Don’t allow your splint to be exposed to sources of heat as the plastic may melt.
- Don’t try to make alterations to your splint. Contact your hand therapist if you have any issues with the splint.
- It is important you keep the normal movement at all joints that are not splinted – this includes other fingers/thumb, wrist, elbow and shoulder
- Don’t do any exercises that the Hand therapist has not shown you
- Don’t force your finger/s to bend
Recovery Period
A tendon will repair by forming a scar, rather like a cut on the skin. However, a tendon takes much longer to heal and remains vulnerable for several weeks.
This is only a guide and may vary according to individual injuries.
0-6 weeks Wear the splint at all times. Do exercises in the splint
6-8 weeks Out of splint for exercises only
8+ weeks Gradually wean from splint. Progress at this point depends on finger position.
12+ weeks Return to contact sports and heavy lifting.
Contact details
Should you require further advice or any problems on the issues contained in this leaflet, please do not hesitate to contact following telephone numbers:
Castle Hill Hospital, Hand Therapy Unit Tel: 01482 622296 (Monday to Friday)
Plastic Surgery Trauma Clinic HRI Tel: 01482 674509
(Daily including weekends and bank holidays)
Your feedback matters to us…
To ensure we deliver a safe and quality service and to help us understand the experience you have of the care you receive from our staff we would value your thoughts about the service you received.
You may be contacted as part of our quality assurance programme which is where we visit our teams and staff and talk to them about the care they provide to our patients or at any time during or after you have needed our services.
To collect this feedback, we would contact you using the registered telephone number we hold in your care record. This feedback will be strictly anonymous and whilst we will share the feedback as part of the process, we will not share any details which may identify you.
We will never ask you any personal questions about your health during these telephone calls.
If you do not wish to speak to us, please say this when we call, we do not want you to feel pressured.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

