- Reference Number: HEY-1301/2024
- Departments: Bariatric Surgery, Upper GI
- Last Updated: 3 January 2024
Contents
|
|
|
|
|
|
|
|
|
|
|
|
|
|
– Pre-operative liver shrinking diet – Bariatric Specialist Nurse |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
– Dumping syndrome |
|
|
|
|
|
|
|
– Pregnancy – Residual excess skin after weight loss – Smoking |
|
– Consent to treatment |
|
|
|
|
|
|
|
|
Introduction
This leaflet has been produced to give you general information about the bariatric (weight loss surgery) service at Castle Hill Hospital. The service is provided by Hull University NHS Teaching Hospitals NHS Trust and is funded under strict criteria by NHS England and Clinical Commissioning Groups. This is based on NICE and local Clinical Commissioning (CCG) policies. There are 4 “Tiers” of weight loss help available to you.
Bariatric surgery is also known as a Tier 4 Service. A patient will need to have met with their GP and found to have a Body Mass Index (BMI) that qualifies for referral directly to the bariatric service for assessment, but this depends on their local CCG commissioning guidelines. If accepted, patients may complete 6 months of assessment and stabilisation and preparation within the service before they can be considered for weight loss surgery. Some practices will have to refer a patient to a medical weight loss service (Tier 3) before a referral to Tier 4 Bariatric Surgery Service can be accepted.
Specific Information about the types of operations and dietary advice are provided in this leaflet. It is not intended to replace the discussion between you and your surgeon / nurse or dietitian. If you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for you.
Is weight loss surgery right for me?
You have probably struggled with your weight for a long time and tried different methods to lose weight. After discussion with your GP, you have requested referral to the bariatric surgery service for assessment as to whether surgery can help you to lose weight and help prevent weight regain. This surgery may also help with other medical conditions, which your surgeon will discuss with you.
What will happen at my first appointment?
You will be invited by letter to attend a specialist bariatric clinic. At the first appointment you may watch a multidisciplinary team video outlining the Tier 4 Bariatric pathway, what type of operations are performed and what is expected of you from a dietetic point of view or you may be asked to watch this at home via a link that we will send you. Following this you will be seen by the consultant bariatric surgeon in person and potentially have a review by a psychological professional, this may be a telephone or a face-to-face assessment.
Lifestyle, emotional factors and historical events can all contribute to weight gain and not being able to lose it. It is a mandatory part of the Tier 4 Bariatric pathway that you will be required to make an appointment for an assessment with a member of the psychology team. A letter will be sent to you after your first appointment with details of who to contact. Evidence tells us that long-term, weight loss surgery results are far more successful when patients are seen and supported by a trained psychological professional if required.
You will meet the bariatric surgeon and they will discuss your surgical options and speak to you about issues which are specific to you, for example, weight history and medical problems. You will be able to ask any questions or discuss any concerns you may have about surgery.
What will happen after my first appointment and how do I prepare for weight loss surgery?
After your first appointment at the specialist bariatric clinic, you will be asked to do the following:
- You will be reviewed by the dietitian. This will help you make changes to your diet so that it is suitable before surgery and also after your operation. To make appointments with the dietitian, you should ring telephone number (01482) 674490. It is essential that you call to make these appointments.
- If your health is not considered safe for surgery, the surgeon may request that you see another specialist for treatment before having your operation. This could be a cardiologist, anaesthetist or psychology professional for example.
- You will be expected to lose some weight before surgery. We understand this may be difficult for you. If you show commitment by following the dietary advice given to you on how to change your diet before to the operation, some weight loss will be possible.
- If you put on weight at any time after your first appointment, or do not complete these steps, we may delay or cancel your surgery. If you do not attend a follow up appointment and fail to notify us to cancel it, you may be discharged back to the care of your GP.
- We would like you to contact the local Bariatric Support Group. Information regarding support groups is on the back of this leaflet provided. We consider engaging with the groups important for all patients. This will allow you to talk to other patients at different stages of the surgical process and then help you make an informed decision about your surgical choices.
Please note clinic follow up appointments can either be face-to-face in the outpatient clinic, via telephone or via video link.
Please share the information in the leaflet with your partner and family (if you wish) so that they can be of help and support. There may be information they need to know if they are taking care of you following your surgery.
Introduction to your diet before surgery
The aim of this is to give you a practical guide to help you make dietary changes so that your diet before surgery is as similar as possible to the diet you will follow after surgery.
This diet will also ensure that you are able to eat foods from each food group and that your diet will be balanced after you have had surgery. By following this diet, you may also find you lose some weight.
It is important to make these changes now so you are ready for what your diet will be like after surgery. In order for you to be considered for bariatric surgery it is important you achieve the dietary changes outlined in this information leaflet. Your dietitian can help you with suggestions on how to make these changes at your individual one to one appointment.
The roll of the dietitian is to support you with making the necessary changes needed to achieve the best possible outcome after surgery.
This will cover:
- The bariatric dietetic pathway
- Expectations around weight and weight loss
- The dietary changes you will need to make and maintain
It is important that you complete all stages of the dietetic pathway and attend all your appointments. If you are not able to attend your appointment, please let us know. If you cancel multiple appointments, you may be discharged. If you fail to attend and do not contact us, you may be discharged.
Frequency of one-to-one appointments will depend on your progress with the dietary changes and how much support you feel you need. Your dietitian will be happy to discuss this with you.
If you have questions or concerns about your diet in-between appointments, please call your dietitian.
Dietitian appointment line: 01482 674490.
Your weight and weight changes
On your first visit to meet the team you will have your weight measured. This is considered to be your starting weight.
It is important that you do not exceed your start weight whilst in the bariatric service as this may delay your progression in the bariatric service. You can track your weight using the weight tracker on page 23 of this leaflet.
By making the required dietary changes it is likely you will lose some weight. This is a positive sign and helps to show readiness for bariatric surgery. If you gain weight this is a sign that you may require additional support in making the required dietary changes, your specialist nurse or dietitian can discuss this with you. If you notice that you are gaining weight or struggling to make and maintain changes, please contact your dietitian who may be able to help.
Once you have been added on to the waiting list for Bariatric surgery it is important to maintain the dietary changes to prevent weight gain as this can lead to a delay in you getting your surgery or your surgery being cancelled. Regular appointments with your dietitian can help reduce this risk. You must book all your 1:1 appointment with dietitian on 01482 674490.
If you do not have scales at home, you may be able to attend your GP surgery for a regular weight check or you may be able to access scales in other places such as your local pharmacy.
Required dietary changes
The changes to your diet before surgery are important as they help you get ready for what your diet will be like after surgery.
1. Start by getting into the habit of having 3 meals a day
This doesn’t have to be typical breakfast, lunch and evening meal but 3 evenly spaced meals throughout the day regardless timings. It is important not to miss meals. Missing meals after surgery can lead to malnutrition. Getting into the habit of routinely having 3 meals per day before surgery will help get you ready for life after surgery
2. Making sure your meals are balanced
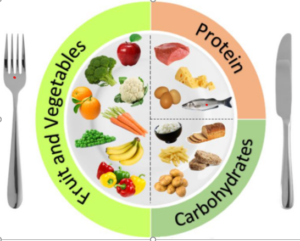
We recommend that your plate should be approximately ½ vegetables (you can eat any vegetables including canned or frozen vegetables), ¼ starchy carbohydrates such as pasta, rice, potatoes, cous cous and bread and ¼ protein such as meat, fish, eggs or vegetarian / vegan alternatives. This should help you to manage your weight before surgery.
3. Getting the right amount of fluid
We ask you to start taking your fluids between your meals. This is to prepare you for life after surgery when it is advisable not to drink with your meals. If you were to drink and eat at the same time after surgery it could make you sick or can push your food through your pouch too quickly causing problems with dumping syndrome, hunger and absorption. Please avoid drinking 30 minutes before a meal and for 30 minutes after you eat. Please see page 17 for more information on dumping syndrome.
Please try to drink a minimum of 2000ml of fluids a day avoiding mealtimes.
You will likely need to carry a water bottle with you all day to make sure you are able to get enough fluid.
Suitable fluids include:
- Water
- Still, sugar free flavoured water
- Tea and coffee (milk and sweetener to taste)
- No added sugar squash
Fluids which are not suitable include:
- Fizzy pop
- Diet fizzy pop
- Fresh fruit juice
- Fizzy alcoholic drinks e.g. larger, cider, sparkling wine, fizzy mixers
- Drinks with added sugar e.g. tea, coffee, high juice
4. Avoid snacking
If you typically have lots of snacks or ‘graze’ on foods throughout the day, it is really important you change this behaviour. Excessive snacking after surgery will mean that you do not lose as much weight and may even regain weight.
If you snack on fruit between meals try to have this straight after a meal instead. Make sure you balance your meal and fill up on vegetables to help you reduce your snack cravings.
5. Know your alcohol recommendations
The guidance advises that:
- To keep health risks to a minimum please follow the government guidelines and do not drink more than 14 units per week. 14 units is equivalent to a bottle and a half of wine or five pints of export-type lager (5% abv) over the course of a week – this applies to both men and women
- Alcohol is high in calories and can contribute to weight gain
- Alcohol is discouraged after bariatric surgery, both in terms of long-term weight loss results and its different effects after this kind of operation.
If you would like advice on how to reduce your alcohol intake, talk to a health care professional who can signpost you to your local services.
6. Try to increase your physical activity levels
The NHS advises that everyone should try to do 150 minutes of moderate intensity physical activity each week this is equivalent to five 30-minute activity sessions. Moderate intensity should mean you are slightly out of breath. If you are not already doing this, please try to increase your activity levels as this will help you to maintain any weight you have already lost and will improve your fitness for surgery.
Don’t worry if your physical health means that you are not able to achieve the 150-minute goal just try to do what you can. You may be able to do chair exercises such as the ones on this NHS website https://www.nhs.uk/live-well/exercise/sitting-exercises/ . Remember physical activity is much less important than dietary changes when it comes to managing your weight and poor mobility does not mean you will not be able to lose weight.
7. Start taking an A-Z multivitamin and mineral
Please start taking an over-the-counter A-Z multivitamin and mineral complete, these are available at pharmacies, health food shops and supermarkets. Taking these before surgery will help to treat any nutritional deficiencies you already have and get you used to taking supplements which are essential after surgery. You will need to take lifelong supplements after surgery.
When will I have my surgery?
After completion of your assessments with your surgeon, dietitian and psychological professional and we are happy with your progress; the bariatric team meets as a multi-disciplinary team (MDT) to discuss your progress. At the MDT meeting we discuss whether you have achieved the below:
- You are making lifestyle changes and losing weight
- You are preparing for the effects of surgery
- You are as fit as possible for surgery
There may be a requirement for you to complete a 6-month stabilisation period and make the recommended diet and lifestyle changes. Should you change your mind about going ahead with surgery it is possible to change your mind at any point.
You will have a further consultation to discuss the MDT’s recommendations. Should any further care, tests or changes be required, we will discuss these with you. If we are satisfied that you are in a position to move forward with surgery, you will then be asked to make an informed decision as to which operation you would like to have.
At this point, your name will be added to the waiting list for your operation, and you will be given a 2-stage consent form (see section on “General Advice and Consent” under specific operation information sheets). This has detailed information on the risks of surgery. We would like you to read and sign each section of this before your operation. It is not possible to tell you exactly how long you will have to wait, but we are committed as a Trust to try to provide your surgery within 18 weeks from the point in which you are put on the waiting list.
Pre-assessment and the pre-operative diet
You will be contacted by the waiting list clerk with a date for your surgery. Your pre-assessment appointment will also be arranged for you which will take place about 4 weeks before your surgery date. At this appointment you will have a full blood, health screen and weight check to make sure you are in good health before your anaesthetic. You will be able to ask any questions you may still have.
Pre-Operative Liver Shrinking Diet
You will be advised when to start the 2-week liver shrinking diet. You will be required to complete this before coming into hospital for your surgery. This diet is very important as it will help to reduce the size of your liver before surgery to ensure your liver does not get in the way of your stomach. This will allow your surgeon the room needed to operate on you successfully. A separate information leaflet will be sent to you explaining the liver shrinking diet. www.hey.nhs.uk/patient-leaflet/bariatric-surgery-pre-operative-diet/. If you have any queries about the diet, please contact the dietitians on 01482 461941.
You will be sent a letter asking you to come to a ward the afternoon before or the day of surgery. If everything progresses as planned, you will spend two further nights in hospital after your operation. You may be asked to attend the day prior to your operation to have a blood thinning injection (low molecular weight heparin, LMWH) and routine blood tests and return the following day to the surgical admissions lounge at Castle Hill Hospital.
You must agree to being followed up in the clinic for at least 2 years after your surgery. This will usually be with the bariatric specialist nurse and bariatric dietitian.
Bariatric Specialist Nurse
You will usually be seen on the day of your operation and the following day by the Bariatric Specialist Nurse. They will discuss any concerns or queries that you may have. The Bariatric Specialist Nurse will contact you at home by telephone within two weeks of your discharge to discuss your progress and any ongoing concerns that you may have.
What is a Roux-en-Y gastric bypass?
A Roux-en-Y Gastric Bypass is a surgical procedure where the surgeon will permanently reduce the size of your stomach by stapling across and dividing the top of your stomach to make a small pouch. This restricts the amount of food and drink which your stomach “pouch” will be able to hold after surgery (the rest of your stomach continues to help digestion even though it doesn’t fill with food anymore). Your stomach can usually hold up to 1500ml (approximately 3 pints) but after gastric bypass this reduces to only 30ml (the size of a large egg).
The second part of the operation involves two joins, the first attaching the small bowel onto the pouch. The second join allows the digestive enzymes to join your food further down which reduces how many calories (but also protein and vitamins) you can absorb. This combination of restriction and reduced absorption makes this one of the most effective weight loss operations available.
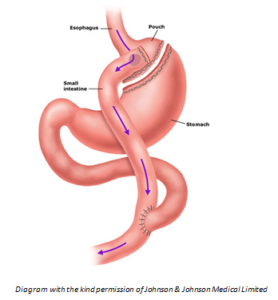
What is a single loop gastric bypass?
A Single Loop Gastric Bypass is a slightly different version of the gastric bypass might be an option for heavier patients.
This involves making a longer, thinner stomach and gastric pouch. This is done by creating only one join with a loop (around 1.5metres) of the small bowel which is where digestive juices (green arrows) mix with the food (red arrows). This is only suitable for certain patients and your surgeon will discuss with you whether this is an option you might want to consider.
Occasionally the small bowel cannot safely reach the stomach pouch to make a gastric bypass because a patient’s weight is too high. This might limit the only alternative operation to a “stomach-restriction” operation (sleeve gastrectomy).
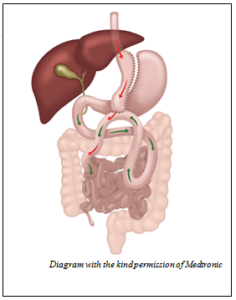
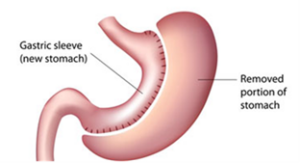
What is a sleeve gastrectomy?
A sleeve gastrectomy is a surgical procedure which permanently reduces the size of your stomach to help you lose weight and maintain weight loss. The surgeon will divide and seal any blood vessels supplying the part of the stomach to be removed. The stomach is then surgically stapled and sealed using a calibration guide tube to measure the size of the stomach tube left behind. This will remove around four-fifths of the stomach permanently. This is known as a restrictive operation. This means it restricts the amount of food / drink that your smaller stomach will be able to hold after surgery. Your stomach can usually hold up to 1500ml (approximately 3 pints) but this reduces to less than 200ml (less than ½ pint).
Removal of this part of the stomach can reduce hunger as it removes cells that produce a hunger-stimulating hormone called ghrelin. Food absorption is not affected by this operation. Absorption of iron and certain vitamins (particularly vitamin B12) can be affected requiring supplementation of these long-term.
How are these operations performed?
These operations are usually completed by “laparoscopic” (keyhole) surgery. Several small cuts (1cm or less) are made to place hollow tube “ports” into the cavity of the abdomen. Long thin instruments and a camera are passed into the “ports” to allow the surgeon access to your organs. The abdomen is temporarily inflated with a gas (carbon dioxide) to create the space in which the surgeon works. It is necessary for you to have a general anaesthetic (be asleep) whilst your abdomen is inflated by this gas. At the end of the operation the gas is released, the wounds are sutured, and you are woken up. If you have a sleeve gastrectomy the stomach is removed through one of the keyhole wounds.
Occasionally internal scar tissue, a large heavy liver or other problems prevent the surgeon performing the operation through keyhole surgery. This may require a larger incision (“conversion to open”) or abandoning surgery altogether for safety reasons.
How much weight will I lose and what effects will it have?
Roux en-Y Gastric bypass and Single Loop Gastric Bypass surgery can achieve over 70% excess weight loss. That is 70% of the extra weight you are carrying over and above your ideal weight for your height.
Sleeve gastrectomy surgery can achieve an average of 65% excess weight loss. That is 65% of the extra weight you are carrying over and above your ideal weight for your height.
This can improve symptoms like fatigue, shortness of breath and improve quality of life such as your energy levels, ability to walk and exercise and may reduce pain in weight bearing joints and the back. In addition, several medical conditions can improve resulting in reduced need for medication. These include:
- Type 2 Diabetes
- High blood pressure
- Sleep apnoea (interrupted breathing during sleep)
- High cholesterol
- Polycystic ovaries
Because you are absorbing less energy (calories) you can occasionally feel faint and a small snack between meals may be needed. It is common to have short-term hair loss (usually in first 6 months) which can be distressing but this recovers and regrows in time. Ensure you discuss your protein intake with your dietitian as this can influence hair loss.
You will be absorbing fewer essential vitamins and after this operation you must take the supplements (see Discharge Medication and Advice section) to avoid complications like thin bones or anaemia.
You must have regular blood tests for the rest of your life and may occasionally need additional iron or vitamin D for example if these levels fall too low.
Can there be any complications or risks?
There are always risks of complications associated with surgery. Overall, less than 1 in 20 patients experience a significant complication. Risks are increased by heavier weight (higher Body Mass Index (BMI)) and medical conditions associated with weight gain.
Immediate and short-term complications:
- Conversion to a conventional open operation (uncommon)
- Anastomosis or staple line leak and peritonitis (uncommon)
- Wound infection (uncommon)
- Bleeding (uncommon)
- Death (very uncommon)
- Incisional hernia (uncommon)
Other complications after surgery
- Heart complications (uncommon)
- Chest infections (uncommon)
- Deep vein thrombosis and pulmonary embolism (uncommon)
Possible Longer-term complications
- Stomach ulcers (uncommon)
- Strictures (uncommon)
- Adhesions (uncommon)
- Internal hernia causing obstruction (uncommon) (Single Loop Gastric Bypass and Roux-En-Y Gastric Bypass only)
- Nutritional deficiencies after surgery
- Less predictable drug and alcohol absorption
- Infertility, contraception and pregnancy in women
- Depression and maladaptive eating (uncommon)
- Weight gain and recurrence of obesity related illness
Single loop gastric bypass only
- Bile reflux (uncommon)
- Inflammation or risk of cancer changes in stomach pouch (very rare)
All of the common and several of the not so common complications have been listed. The list is not exhaustive. If you have any of these after your operation, you may require an emergency re-operation in order to correct the problem or longer stay and treatment in hospital.
The surgeon will also discuss with you your estimated mortality rate from this kind of surgery. This varies greatly between each patient. Everyone has different risks based on their weight and other illnesses. The average risk to life is around 1 in 300.
Your stay in hospital after weight loss surgery
When you have had your surgery, you may spend some time within the recovery area of the operating department. They make sure you are not in pain and awake enough to be transferred to the Critical Care Unit or a High Observation Bed where nursing staff can monitor you carefully, usually for your first night after surgery. You will have your blood pressure and other vital measurements taken regularly throughout the night.
When you need to use the toilet, the nurse will help you get up to go if needed. A catheter is NOT routinely needed. It is important to start moving and walking as soon as possible after your operation, to reduce the chance of blood clot or chest infection developing. You will be wearing compression stockings and/or mechanical compression boots to encourage circulation after surgery. You may have a surgical drain/tube placed near the wound to remove blood or fluid. This will usually be removed by the second day following your surgery.
Please make sure your friends and relatives are aware you may not be on the ward for your first night after surgery. It is normal to spend your first night after surgery on the Critical Care Unit or a High Observation Bed.
You will be transferred to the ward and stay a further 1-2 days
Post-operative swallow test
Shortly after your operation, on the first or second day usually, you may have a contrast swallow test. This is an X-ray test where you will be asked to swallow some colourless liquid (contrast), which then passes through your stomach and bowel and can be seen on X-ray. It will show the doctors if there are any leaks or blockages. Once this is confirmed to be normal, you will be able to start drinking and eventually start your diet plan. Until this test is completed, you will often have IV fluids (drip), to make sure you have enough fluid in your body and therefore do not get dehydrated.
Eating and drinking after weight loss surgery
You may not have anything to eat or drink until after your X-ray swallow test. The doctor will inform you when you can start to drink fluids. Until this time, you will have fluids to hydrate you through a drip. You may get a very dry mouth. The nurses will offer you mouth washes, and you will be able to gargle as long as you do not swallow anything.
When the results of your swallow test are known, you will be able to start drinking, very slowly at first. At mealtimes you will also be able to start to eat a liquid meal. You will not be discharged until you are managing to eat and drink successfully.
The specialist dietitian will have already discussed the post-operative diet with you in detail and provided you with a written diet plan for the weeks after surgery. They may also see you on the ward. Your diet will gradually build up to more solid food. You must avoid drinking fluids at the same time as food to avoid vomiting and dumping syndrome (see below).
Use the diet plan as a guide but it will be trial and error over what food you can manage at first and it takes time to get used to feeling fuller more quickly. The first 3 months can be difficult, and it is not uncommon to occasionally feel sick or regurgitate food, but this should settle completely with time.
If you are unsure about your diet or fluids, ask to speak to the dietitian before you are discharged from the ward, or ring up for advice (01482 674490) if you are in-between outpatient appointments. Do not struggle on unnecessarily; our specialist dietitian/nurse will always be happy to advise you.
Dumping Syndrome
This is an unpleasant set of symptoms including feeling sick, weak, faint, sweaty and diarrhoea. It is where the food in your stomach is either too liquid and sugary or too quickly washed into the small intestine through the join. This is why it is vital to never have sugary drinks. You should also avoid drinking liquids 30 minutes before or 1 hour after a meal. (More common in Roux-En-Y Gastric Bypass and Single Loop Gastric Bypass)
Discharge and medication advice
You must take the discharge medication below as outlined on your discharge letter:
- Vitamin D 2000-4000 international units dependent Vitamin D result (with the ideal Vitamin D range being ≥ 75 nmol/L).
- A multivitamin A-Z complete with iron (e.g., Forceval® or other alternatives are available, please seek advice from your pharmacist).
- Please note: Some patients may require calcium and Vitamin D. Ensure you leave a gap of 2 hours between taking the Vitamin D and calcium combined tablet and the A-Z multivitamin.
- Lansoprazole 30mg (oro-dispersible) once daily for 4 weeks
- Low Molecular Weight Heparin injections (a total of 7 days including your inpatient stay)
- Iron supplementation may or may not be required
- 6 weeks following your surgery, your surgeon or specialist nurse may recommend that your GP commences vitamin B12 injections every 3 months or a daily tablet of Cyanocobalamin, as your absorption of this vitamin is affected by weight loss surgery.
- Ensure that you wear your anti-embolic compression stockings (TEDS) for 2 weeks after your surgery.
- You can shower but not bathe for 1 week after your surgery.
- Ensure that if you have any dressings, you keep them clean and dry for 5 days and then remove the dressings. Most wounds are closed with absorbable stitches. If you have any bleeding, redness, swelling or excessive pain, please contact the discharging ward, Bariatric Specialist Nurse or your GP.
- Your drain site may ooze for few days after discharge, but this should stop within 2 to 3 days. Additional dressings will be provided by the ward if needed.
- Ensure that you have requested a ‘fit’ note from the ward doctor if you require one. You should expect to return to work after 2 to 4 weeks.
- Regular blood tests will be required over the 2 year follow up period and occasionally, additional supplements will be needed if levels fall.
- Ensure that you have your dietetic post-operative diet sheets before you are discharged.
- Check your car insurance policy before driving. You can usually drive when you can safely perform an emergency stop and turn to look at your blind spot usually after 1 to 2 weeks providing you are not taking any medication that may affect your ability to drive.
- Do not do any abdominal/heavy exercises for at least 6 weeks post- operative.
- You may resume intimate activities when you are ready.
- If you become constipated, before seeking further advice ensure that you are drinking at least two litres of water daily between your meals.
- Please speak to your doctor for advice if you intend to fly within the next few months. See also http://www.caa.co.uk/Passengers/Before-you-fly/Am-I-fit-to-fly/Guidance-for-health-professionals/Surgical-conditions/
Exercise before and after surgery
You should walk daily straight away. After 3 weeks you should try to increase your activity with something that is realistic and accessible. Gardening, housework, swimming and dancing are all popular and effective ways to get your heart rate up. Strength exercises such as squats (crouching down) and shoulder shrugs are simple ways to maintain posture and upper body strength. Those with limited mobility should attempt chair-based exercises wherever possible. You can attend the gym after 3 weeks but avoid heavy weights for 6 weeks.
What must I do to ensure my operation will work long term?
Any weight loss surgery can fail to help you lose weight if vital lifestyle changes are not made before and after surgery. This can cause weight re-gain if lifestyle changes are not followed. Only you can make these changes. This is why we prepare you for surgery over a period of months to ensure you are making the correct changes in diet and exercise to ensure it will succeed. If we feel that you are not able to make these changes (which is hard work) then you may not be offered surgery.
Examples of essential changes are:
- A diet consisting of regular 3 meals per day that is low in sugar
- Avoiding drinking liquids with meals
- Avoiding snacks like crisps and sweets or sugary juices/drinks
- Increased activity (see section on “Exercise Before and After Surgery”)
- Consider other ways to improve your mood or relax instead of relying on food
Important points about weight loss surgery
Pregnancy
Losing weight can result in increased fertility. Female patients having weight loss surgery may wish to have children but must avoid falling pregnant ideally in the first 18 months after surgery. The growing baby may be harmed by a lack of nutrition during this time. Different types of contraception (e.g. coil, barrier methods) should be considered after this surgery as the reliability of the contraceptive pill may be reduced.
If you do become pregnant following weight loss surgery, please contact us for further advice.
Residual Excess Skin after Losing Weight
Loose excess skin is not uncommon after weight loss surgery and will happen in the majority of cases. The bariatric service does not perform surgery for excess loose skin. If this becomes a future concern, you should discuss this with your GP. It is unusual for the NHS to fund such excess skin removal surgery, and this is only by special agreement after an application by your GP. Many patients are not concerned by loose skin but for those who are, a private consultation with a plastic surgeon may be something you wish to consider but it is most likely you will need to pay for this. We would advise that you do your own research in to the impact of excess skin as this can affect your both psychically and psychologically. We advise that you do your own research. You will be able to find images of people with excess skin on the internet following their Bariatric surgery.
Smoking
Smoking is a serious health risk, and you must stop smoking if you wish to have weight loss surgery. Smoking increases overall risk of complications and the specific risk of ulcer formation in the stomach. This can lead to long-term pain, vomiting and even internal leaks or perforation. Smoking cessation services are available through your GP.
Contact Information:
Claire Hunt, Bariatric Specialist Nurse
01482 624309 (Answerphone available)
Email: hyp-tr.bariatricnurses@nhs.net
Dietitian appointment line – 01482 674490
You must telephone to book all dietetic appointments within 1 month from your latest dietetic appointment. If you do not comply with this you may be discharged back to the care of your General Practitioner and this discharged from the Bariatric Pathway.
OWLSS
Weight Loss Support Group (Led by volunteers not NHS staff).
Virtual Meetings – Dates and times available on Facebook page.
To be invited to the Facebook group please contact the below email advising you have attended your first appointment:
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Bariatric Department on Tel no: (01482) 624309
For Dietetic advice contact (01482) 674490
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

