- Reference Number: HEY144/2023
- Departments: Paediatric Medicine
- Last Updated: 31 August 2023
Introduction
This leaflet has been produced to give you general information. Most of your questions should have been answered by this leaflet and it is not intended to replace the discussion between you and the healthcare team, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
Why are Hip Spicas used?
Hip spicas are used to keep the hip joint and legs stable, immobile and in the most appropriate position for bone, tendons and ligaments to grow.
For example: following treatment to correct hip dislocation or a fractured femur.
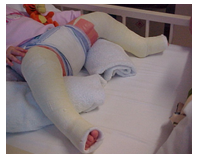
Where is the Hip Spica applied?
Hip spicas are made by applying plaster of paris or lightweight fibreglass, over some wadding.
It will be applied in theatre following hip surgery and whilst your child is under a general anaesthetic.
Any further changes of the Hip Spica, can be done either under a general anaesthetic or in fracture clinic, with or without sedation.
Do they hurt?
The Hip Spica itself should not cause pain but they are cumbersome and at times uncomfortable. Following surgery your child may experience some pain, which will be assessed and appropriate pain relief will be given.
Hip Spica Care
Fibreglass casts dry in a couple of hours however plaster of paris takes up to 48 hours to dry. During this time:
- Do not write on, press or bump the plaster cast. This may cause an indentation inside causing pressure on the skin
- Do not push things down the inside of the cast
- Do keep the Hip Spica and the wadding dry
- Do check circulation to toes
- Do look for swelling, changes in colour (blue or pale)
- Do apply socks if the feet are cold to touch
- Do check skin around groin, bottom and back for excess tightening
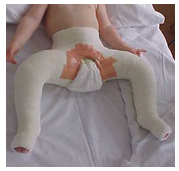
Your Spica will be ‘sleeked’ (Sleek is a waterproof tape that is applied to the edge of the Hip Spica). In hospital, you will be shown how to apply further sleek, which will help prevent urine and faeces soaking into the plaster causing discomfort and odour. Check the tape remains secure around the edges of the plaster.
For children in nappies, parents will be shown how to apply a double nappy system. Frequent nappy and/or pad changes are vital to keep the cast and wadding clean and dry. Nappies should be checked and changed at least every 2 hours during the day and at least twice during the night.
If your child produces excess moisture during the night as long as they are drinking lots of fluids in the day it may be a consideration to reduce intake of fluids 2 hours before bed.
If your child has been potty-trained prior to admission, they will need to sit upright on a potty or bedpan to prevent soiling.
The hip spica will smell if soiling is not avoided.
- You will be shown a safe way to lift your child, this should be done by supporting under the Hip Spica itself.
- Positioning your child in a semi propped up position using a beanbag or pillows. This will allow gravity to drain moisture away. Regular 2-3 hourly change of sitting position from front to back and side to side will help relieve pressure on the skin and allow air to circulate around the plaster.
- Check the skin around toes, spine, tummy and sides for redness or signs of pressure. You may need to change your child’s position to relieve this pressure.
- To help dry out any moisture around the nappy area your child may be nursed without a nappy for short periods. A barrier cream may be used if necessary.
- Ensure your child’s safety at all times especially when laid on their tummy. You may find a beanbag is useful for positioning your child.
- Meal times can be messy, please ensure the plaster cast is covered.
- Although your child may not be immersed in baths, they still need a daily wash. The skin may become itchy and baby lotion may be used to relieve this.
- Ensure toys are within easy reach of your child.
- Provide a variety of activities to prevent frustration and boredom
- If your child attends school, try to discuss your child’s educational and mobility needs with them prior to admission.
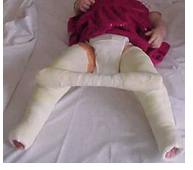
Transport and Mobility
Getting out and about will be one of the biggest problems you will encounter and it is important for you and your child’s wellbeing to be able to do so.
Prior to your child’s admission to hospital you should ensure that you have a suitable car seat and pram / buggy to accommodate the Hip Spica.
The registered charity, called ‘STEPS’ has a help-line with an updated list of commercially available car seats. The hospital is unable to provide car seats or buggies for use at home.
If your child needs a wheelchair whilst in a Hip Spica, we will contact our Occupational Therapist during your admission. She will come and measure your child, and make every effort to find an appropriate chair. This may involve accessing a local wheelchair service in the community.
Car Seat Loan – Hip Spica Options
In Car Safety Centre
https://incarsafetycentre.co.uk/services/loanscheme
The in Car Safety Centre Loan Scheme allows parents to loan a seat for the period (normally up to 4 months) while your child is fitted with such a device. The seat manufactured by Britax Romer, is a standard seat and modified for this purpose. The modification requires the replacement of the original crotch strap with an extended one. Additional padding is also added. The cost to have the loan of the seat is £220, which includes a £75 deposit, refunded when the seat is returned.

Maxi Cosi
https://www.maxi-cosi.co.uk/c/happy-hips-service
The Maxi Cosi Opal HD gives extra back support and space for the legs that’s so vital for children with hip dysplasia. Parents in Europe can borrow it through our Happy Hips service, and feel confident knowing their child is travelling safely.
This service works based on an initial deposit of £120. For every month (or part month) you require the seat we deduct £10, with any remaining deposit being refunded to you upon safe return of the seat.

When your child has been diagnosed with a hip condition you may come across some names which are unfamiliar to you. Listed below are some definitions to help you understand what you are being told at the hospital:
ORTHOPAEDICS – The branch of medicine that deals with the bones, joints and the soft tissues of the limbs and spine
ABDUCTED – To hold legs apart, away from the centre line
ACETABULUM – the cup shaped socket of the hip joint
BILATERAL – Affecting both sides
DISLOCATED – When a joint is out of place
DYSPLASIA – Not properly formed
FEMUR – Thigh bone
IDIOPATHIC – Cause unknown
TENOTOMY – The cutting of a tendon
Should you require further advice on the issues contained in this leaflet, or have any concerns regarding your child’s Hip Spica, please do not hesitate to contact any of the following:
Fracture Clinic HRI – 01482 674378
Plaster Room – 01482 675731
Acorn Warn HRI – 01482 382703
Paediatric Pre-op – 01482 382647
Paediatric Assessment Unit – 01482 674455
Woodlands Trust – 01482 674465
www.steps-charity.org.uk can be contacted on 08717 170 045
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats your child, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to your child. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your child’s condition, the alternatives available for your child, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about your child
We collect and use your child’s information to provide your child with care and treatment. As part of your child’s care, information about your child will be shared between members of a healthcare team, some of whom you may not meet. Your child’s information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide your child with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your child’s doctor, or the person caring for your child.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about your child. For further information visit the following page: Confidential Information about You.
If you need information about your child’s (or a child you care for) health and wellbeing and their care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.
