- Reference Number: HEY1347/2026
- Departments: Orthopaedics
- Last Updated: 28 February 2026
Introduction
This leaflet has been produced to give you general information about your injury. We understand you may not have seen a clinician face to face in fracture clinic however; this leaflet should answer most of your questions. If after reading it, you have any concerns or require further explanation, please do not hesitate to contact the fracture clinic team. Contact details are available at the end of this leaflet.
What is an acromioclavicular (AC) joint injury?
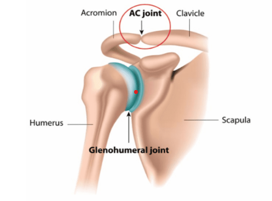
The acromioclavicular Joint or AC joint is a joint at the top of the shoulder.
It is the junction between the acromion (part of the scapula that forms the highest point of the shoulder) and the clavicle (collarbone).
The AC joint is injured by a direct fall onto the point of the shoulder. The shoulder blade (scapula) is forced downwards and the clavicle (collarbone) appears prominent.
The degree of injury to the joint is classified by the amount the joint is displaced and the injury to the ligaments which support the AC joint. There are six grades.
- Grade 1 and 2 are sprains of the ligament with no or minimal displacement.
- Grade 3 is a complete tear of the ligament with minimal displacement.
- Grades 4 to 6 are more complex and the clavicle or collarbone become displaced.
Traditionally the grade determined the treatment. However, the evidence for this is poor and nowadays, we treat according to the symptoms of pain and functional limitations.
These injuries normally takes around 6 weeks to heal. The pain can be quite bad for the first few weeks and soft tissue injuries can persist for up to 3 months.
It is important to note that your AC Joint may be more prominent than before your injury. This may be permanent but will not affect your range of movement.
How should it be treated?
During your attendance at the Emergency Department, your shoulder may have been x-rayed and depending on the result of this, you will have been referred either to physiotherapy or to the Virtual Fracture Clinic (VFC).
If you have been referred to physiotherapy then this leaflet gives you some basic advice and exercises to complete while you await a physiotherapy appointment.
If you were referred to the VFC, an orthopaedic consultant will have viewed your x-rays and confirmed that you have an injury of the AC joint. The management of this injury is discussed below. Some patients will require a follow up at 3 weeks however in most cases the consultant will discharge to the care of the physiotherapy team.
In either case, a sling can be worn for comfort only for around 3 weeks (if provided) to allow the soft tissues to heal. If you find your pain has reduced significantly then you can wean out of the sling before the 3-week stage.
In the early stages you may find that pain is an issue and so we advise simple pain relief, which can be bought over the counter. If you have allergies or conditions, which prevent the use of pain-relieving or anti-inflammatory medication, please seek advice from your doctor or a pharmacist.
In the first 72 hours, using ice packs on the injured area may help with pain. It can be applied for 10 to 15 minutes every 2 to 3 hours. This will also help to reduce any swelling.
There are many different ways in which ice can be applied however crushed ice, in the form of frozen peas for example, is the most effective. Whichever method you choose it is important that you wrap the ice in a damp towel, in order to prevent it from ‘burning’ the skin.
Remember however, you should:
- Only use an ice pack on areas that have normal skin sensation i.e. where you can feel hot and cold
- Not apply ice to an open wound
- Not apply an ice pack to an area that has poor circulation
- Check the skin every five minutes and stop using it if:
- the area becomes white, blue or blotchy
- the area becomes excessively painful, numb or tingles
Dressing
It is easier to use front button shirts and pull-up trousers with an elastic waistband in the first few weeks. When dressing put the injured arm into sleeves first and when undressing take the un-injured arm out first, followed by the injured arm.
Armpit Hygiene
To wash under your arm. Gently take your arm out of the sling and straighten your arm. Now lean forwards slightly so that your arm hangs slightly away from your body. You should then be able to wash and apply deodorant.
Driving
You will not be insured to drive whilst you a wearing a sling. It is always good to check with your insurance company however, we advise it should be safe to return to driving when:
- You are no longer using the sling
- You can comfortably grip the steering wheel, move the gear stick, pull up the hand brake and activate the indicators
- You can perform an emergency stop
Can I do any exercises to help?
You can use your arm as pain allows but you should not perform any exercises above shoulder height for 2 weeks.
The hand, wrist, elbow and neck can be moved gently through their full range as comfort allows from day one of your injury. This will prevent stiffness developing in these joints while your shoulder is in a sling. Below is some guidance on the exercises you can do, all of them can be practised 3 to 4 times per day.
Finger flexion and extension: Whilst in your sling make a tight fist with your affected hand and now spread your fingers out as far as possible. Repeat 10 times
Wrist flexion and extension: Whilst remaining in your sling support your forearm with the unaffected arm. Using your wrist only, move your hand down towards the floor.

Hold the stretch for 10 seconds
Now move your hand towards the ceiling. Repeat 10 times each direction
Elbow Flexion/Extension: Remove the arm from the sling and straighten it
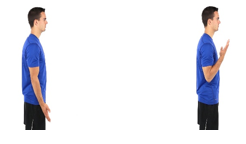
Now bend the elbow as much as possible
Repeat 10 times slowly in each direction
Neck rotation
 Sit upright in a chair and turn your head and neck as far to left as possible. Hold 5 seconds and return to start
Sit upright in a chair and turn your head and neck as far to left as possible. Hold 5 seconds and return to start
Now repeat to the right as far as possible. Hold 5 seconds to return to the start
Repeat 10 times slowly in each direction
Neck side flexion
 Sit upright in a chair and drop your ear down to your left shoulder as far as possible without lifting the shoulder. Hold 5 seconds and return to start
Sit upright in a chair and drop your ear down to your left shoulder as far as possible without lifting the shoulder. Hold 5 seconds and return to start
Now repeat to the right as far as possible. Hold 5 seconds to return to the start
Repeat 10 times slowly in each direction
At 2 weeks or earlier if your pain is under control, you can take your arm out of the sling to start regular pendular exercises. Do not feel you have to wean off analgesia too soon, as it is better to regain some movement first.
Pendular exercises
 Rest your unaffected arm on a table and let the affected arm hang down freely
Rest your unaffected arm on a table and let the affected arm hang down freely
Try to write each letter of the alphabet using this arm
Do not force the movement. Once complete reapply the sling for comfort
All photos with kind permission of ©Physiotec™
Do I require a follow-up?
Do I need to be referred to Physiotherapy?
If the fracture clinic team feel you need to be seen by the Physiotherapy team, you will be directly referred to physiotherapy from fracture clinic and if this is the case, you will have been informed of this in your telephone call, following your Virtual Fracture Clinic appointment. You will receive a letter or phone call to book this appointment within 2 weeks of the referral being made.
If you have not received an appointment within this time, please contact the physiotherapy department on tel: 01482 674880 between the hours 8.00am to 4.00pm Monday to Friday. If there is no answer please leave a message and your call will be returned with the same working day.
Most of the time however, a referral to Physiotherapy is not needed, but if you have any concerns, are unable to follow the advice in this leaflet, or if you still have reduced movement, strength or function, East Riding GP patients can contact the East Riding MSK Physiotherapy service on tel: 01377 208300. Alternatively you can complete a self referral form on https://www.chcpmsk.org.uk/self-referral-form-introduction
Hull GP patients should call the fracture clinic number in the information below.
Do I need a Fracture Clinic follow up appointment?
Some patients will require a fracture clinic follow up at 3 weeks, you will again have been notified of this when you were called by the fracture clinic team. If a follow up is not required you will have been placed on a Patient Initiated Follow Up (PIFU) pathway. This means you will not have another appointment to be seen in fracture clinic.
If, however you have any problems or further queries relating to this injury within the next six weeks, you can contact us on tel: 01482 674378 during clinic hours 9.00am to 4.30pm Monday to Friday. Please do not choose an option and when prompted leave a message if there is no answer and we will aim to get back to you within the same working day. If you have not needed to contact us in the six weeks after your injury, you will be discharged and should seek advice from your GP.
When should I start increasing my activity?
Repetitive shoulder movements and lifting objects heavier than a glass of water should be avoided to begin with. However, as your movement improves and pain reduces, little by little you can increase the amount of weight that you are able to lift. Progressing quickly from lifting a glass of water to a heavy shopping bag for example would not be advisable, as is likely to result in overloading of the soft tissue and could consequently lead to further injury.
If you participate in an active hobby then it is advisable that you do not return to this until you have full strength and full range of movement. A physiotherapist will be able to advice you regarding this.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

