- Reference Number: HEY1085/2024
- Departments: Neurology and Neurosurgery, Physiotherapy
- Last Updated: 31 January 2024
Introduction
This leaflet has been produced to give you general information about your condition and your treatment. Most of your questions should be answered by this booklet. It is not intended to replace the discussion between you and your physiotherapist, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for you.
What is a spinal fracture?
Following you recent trauma or accident, your x-rays and other scans have shown that there is a fracture (broken bone) in your spine. This may look something like this on x-ray and your physiotherapist will show you your imaging at your appointment if you would like to see it. Most fractures take between 6 and 12 weeks to heal. This does not mean all of your pain will be gone by this time but it does usually start to feel a bit better about 4 to 6 weeks after the injury.
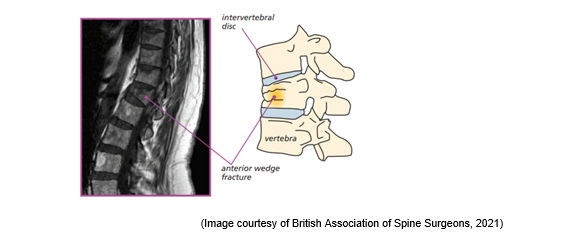
How will my fracture be looked after?
Most spinal fractures are managed conservatively, this means that the fracture will heal naturally by itself over time. Although the fracture will heal by itself, it can be painful, especially in the early weeks after the injury. Sometimes, you will be asked to wear a brace to support the bone as it heals. This will be discussed with you if one is needed.
Pain relief
As you recover from your fracture you may need to take some pain relief to help manage the discomfort. It would be better for you to take medication that allows you to gradually get back to your daily routine than to struggle and become more inactive. Some over the counter pain medication (those that do not need a prescription) can be helpful if you are able to take it and you take it as per the instructions. Please discuss this with your pharmacist. If over the counter pain relief is not helping or you cannot take it for any reason then please speak to your GP who will be able to help decide the best pain relief for you to take.
You may find a hot water bottle or wheat bag many help to relieve any muscle spasm and make you feel more comfortable. As long as you do not have any unhealed cuts or wounds on your back this is okay for you to try.
Do I need to wear a brace?
Not all people who have a spinal fracture need to wear a spinal brace. This decision will be made on an individual basis based on the type of fracture you have, the location of the fracture and any other medical problems or injuries. If you do need to wear a brace it is usually worn for about 8 weeks. Sometimes it can be advised for longer than this and this will be decided after your follow up x-rays or scans. If you do need to wear a spinal brace you will be provided with training on how to use it and a separate booklet about how to manage the brace. If you have any questions or concerns about the brace please contact the neurosurgical physiotherapy team on tel: 01482674333.
Can there be any complications or risks?
Whilst most fractures do go on to heal on their own, occasionally a different treatment option is needed. This could include adding a brace if you are not already wearing one, considering a vertebroplasty (where some cement is injected into the bone to help it heal) or an operation. If any of these are needed this will be discussed with you at your appointment so that you can make an informed decision about your care.
What can I do whilst I am recovering from my fracture?
Please read the information leaflet. Share the information it contains with your partner and family (if you wish) so that they can be of help and support. There may be information they need to know, especially if they are taking care of you whilst you recover from your spinal fracture.
Whilst you are recovering from your spinal fracture there are some general ‘do’s and don’ts’ to follow.
Things you should do
- Walking is a great way to maintain your activity and fitness levels whilst you recover from your spinal fracture. Try and go for a walk each day. There is no set distance or time you need to walk. Do what feels comfortable and build this up gradually over the weeks ahead.
- It is fine to continue with normal daily activities, for example light household chores. However, you should avoid heavier jobs such as hoovering for now.
- It is important to pace your activity as you recover from your fracture to help keep your pain level balanced.
- Change your position regularly, ideally about every 20 to 30 minutes as this will help to prevent too much stiffness building up in your back. For example; stand up beside your chair each time the adverts come on the television or spend 20 minutes laid on the bed whilst you read.
- As a general rule ‘little and often’ is usually the best way to approach any activity as you recover.
- You may sleep in any position which is comfortable for you. However, if possible, do try and avoid sleeping curled up as this will mean your spine is in a bent position for a long period of time (don’t worry if you wake up in this position). Using pillows to support you in bed (as in the pictures) might help make you more comfortable.

(Physio Tec)
Things you should not do
- Avoid lifting anything heavy. A rough guide is not to lift anything heavier than a kettle filled with water.
- Do not twist your back. You should particularly avoid repeated twisting of your back for now.
- Try and avoid bending your back too much. It is ok to bend to put on your socks and shoes, but you should avoid activities which mean you have to bend repeatedly; for example, weeding the garden.
- If you are wearing a spinal brace you MUST NOT drive as your ability to turn and check your blind spots will be restricted. If you are not wearing a brace you may be able to drive depending on your pain and medication requirements. We advise that you inform your insurance company about your injury before considering driving a vehicle.
Work
It is likely that you will need to take some time off work straight after your fracture has happened. When you go back to work will depend on several things, including the type of work you do, how far away from home your job is and whether you or your employer are able to alter your role to support you as you recover from your fracture. It is usually a good idea to return to work on a phased basis, building up your hours or increasing your duties over a period of a couple of weeks as your spine recovers.
What follow-up will I have?
You will be followed up at Hull Royal Infirmary under the care of the neurosurgical team. You have been assigned a neurosurgical consultant to oversee your care but you will not routinely be seen by the doctor at these appointments. At your appointments you will be seen by a specialist physiotherapist who will assess you and discuss any questions you have about your recovery. Your x-rays will be reviewed by the medical team and a plan made for what happens next. Most people have 2 follow up appointments, one at about 2 weeks after your injury and one at about 8 weeks after the appointment. Sometimes you will need extra appointments, if this is the case we will discuss this with you at your appointment.
Information about weaning from your brace
You will have been wearing your brace daily for a number of weeks to support your back and prevent movement around the fracture site. At your final appointment you will be advised about whether you can start to wean from your brace.
It is advised that you remove your brace gradually to prevent sudden strain on your back. Your physiotherapist will have recommended you gradually decrease the time spent in your brace to aid strengthening of your spinal muscles. This should be done daily over a course of 1 to 2 weeks.
It is completely normal to feel stiff initially in the affected part of your spine, this will improve as your activity levels increase which could take a few weeks.
Returning to activity
Low impact exercises such as swimming, cycling and yoga are recommended. It is advised that you begin with a very short period of exercise and build up gradually so that you can monitor whether the exercise feels helpful or not. For example, swim a few lengths and increase by a length or 2 each time you swim, or cycle for 10 minutes and add a couple of minutes each time you ride your bicycle. Returning to more high impact activities, for example, horse riding or mountain biking, should be discussed on an individual basis at your follow-up appointment.
It is normal to experience some discomfort when you increase your activity levels or start a new exercise. Usually this is just the muscles and joints getting used to the new movements and adjusting. If you experience severe pain after an exercise please stop until the pain settles and then gently reintroduce the activity.
After you have had a fracture in your spine, you may feel worried about returning to activity. This can lead to you restricting your movement or moving in an abnormal way. Avoiding normal movement after the fracture has healed may cause your pain and stiffness to be worse and so it is important to try and move as naturally as possible. Feeling anxious about your movement can increase the tension in your muscles which in itself can be painful. If you are feeling anxious it may help to try a relaxation exercise such as the one below to help reduce the tension in your body. This can be done at any stage in your recovery.
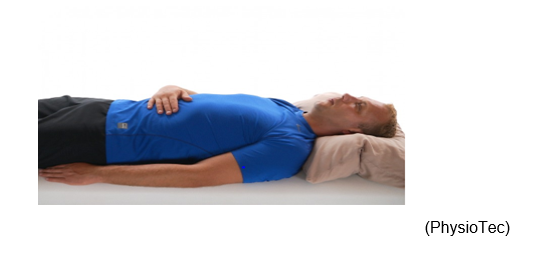 Lying on your back, head on a pillow and one hand on your stomach. Breathe in, for a count of 4 seconds, to inflate your abdomen under your hand, then breathe out. Using this exercise often helps decrease muscle tension and relieves pain.
Lying on your back, head on a pillow and one hand on your stomach. Breathe in, for a count of 4 seconds, to inflate your abdomen under your hand, then breathe out. Using this exercise often helps decrease muscle tension and relieves pain.
There are also some gentle exercises which may help you as you recover from your spinal fracture, again, you can start these straight away:
Pelvic tilt
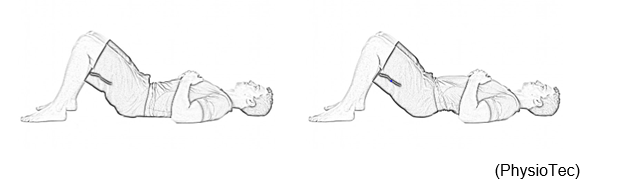
- Lie on your back with your knees bent.
- Activate your lower abdominal muscles by bringing your belly button inward and by activating your pelvic floor muscles slightly (squeeze as if you are trying to stop yourself having a wee).
- Maintain a steady breathing while tilting your pelvis and flattening your back to the ground.
- Return slowly to the starting position.
- Next, arch your back, tilting your pelvis in the opposite direction and your lower back will move away from the surface of the bed/floor.
Repeat up to 10 times, 2 to 3 times per day.
Should blade strengthening for posture
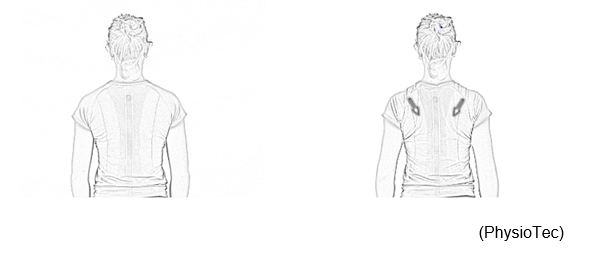
- Stand or sit with your arms resting comfortably in front of your body.
- Straighten the back.
- Pull your shoulder blades together slightly, as well as try to push the shoulder blades down.
- Hold the position for up to 10 seconds
Repeat this regularly throughout the day.
If these exercises cause significant pain which does not settle within 30 minutes of completing them, try and reduce the number of repetitions or length of the muscle contraction. If this does not help, please discuss with the physiotherapist at your appointment.
Important information to be aware of
Please be aware of these symptoms of a rare but serious back condition. If you have any of these symptoms you should go to your nearest Emergency Department straight away:
Common back pain
Many patients have a combination of back pain, leg pain, leg numbness and weakness. These symptoms can be distressing for you but do not necessarily require emergency medical attention. A rare but serious back condition, Cauda Equina Syndrome, can lead to permanent damage or disability and will need to be seen by an Emergency Specialist Spinal Team.
Cauda Equina Syndrome Warning Signs (Any combination seek help immediately)
- Loss of feeling/pins and needles between your inner thighs or genitals.
- Numbness in or around your back passage or buttocks.
- Altered feeling when using toilet paper to wipe yourself.
- Increasing difficulty when you try to urinate.
- Increasing difficulty when you try to stop or control your flow of urine.
- Loss of sensation when you pass urine.
- Leaking urine or recent need to use pads.
- Not knowing when your bladder is either full or empty.
- Inability to stop a bowel movement or leaking.
- Loss of sensation when you pass a bowel motion.
- Change in ability to achieve an erection or ejaculate.
- Loss of sensation in genitals during sexual intercourse.
Useful resources
Here is a link to the Royal Osteoporosis Society and Vertebral Fractures Study information on spinal fractures which you may find helpful as you recovery from your spinal fracture. These resources have been developed for people who have a spinal fracture due to osteoporosis. However, much of the information will also be useful for anyone who has a spinal fracture. The link is below or you can scan the QR code to be taken to the website. If you do not have access to the internet, please ask your physiotherapist for a printed copy of the resources at your appointment.
Royal Osteoporosis Society – https://theros.org.uk/information-and-support/osteoporosis/spinal-fractures/
The Vertebral Fractures study – a guide to diagnosis for patients and carers.pdf (bristol.ac.uk)

