- Reference Number: HEY1033/2024
- Departments: Maternity Services
- Last Updated: 29 February 2024
Introduction
This leaflet has been produced to give you general information about sepsis during or after pregnancy. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and your midwife or doctor, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team.
What is sepsis?
The purpose of this leaflet is to give you some information and guidance on what to do if you think you have an infection during or after your pregnancy.
Infection in pregnancy and/or after your baby’s birth should never be ignored. Some infections can progress to a more serious situation where the infection spreads to the blood stream and occurs throughout the body, this is known as sepsis. Sepsis is the reaction to an infection in which the body attacks its own organs and tissues. If left untreated sepsis can lead to shock, multi-organ failure and death. Whilst most women do not suffer from infection or sepsis during or after pregnancy, if they do it needs to be recognised and treated quickly.
Signs of sepsis 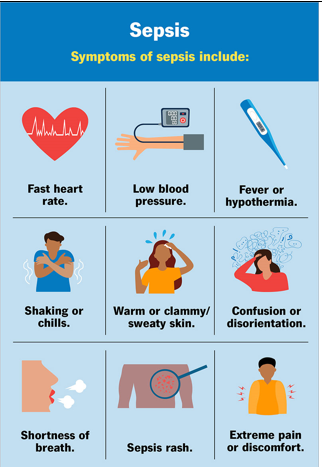
The first signs of sepsis are usually a rise in your temperature, heart rate and breathing. You may also feel unwell; have chills and flu-like symptoms and a worrying pain in your tummy and/or diarrhoea. This can progress very quickly and rarely this can progress to a potentially life threatening condition known as sepsis.
Slurred speech or confusion
Extreme shivering or muscle pain
Passed no / very little urine in a day
Severe breathlessness
I “feel like I might die”
Skin mottled or discoloured
How can infection in pregnancy or after childbirth be prevented?
Good personal hygiene helps. This can include; daily showers/baths, proper hand washing and drying, perineal hygiene to include keeping the perineal area (between the vagina and back passage) clean, dry and frequent changes of maternity/sanitary pads. It is important to wash your hands before and after going to the toilet and changing maternity/sanitary pads.
When am I more likely to get an infection or sepsis?
Sepsis may happen in pregnancy or after your baby is born. The risk of getting an infection is increased in the following circumstances:
- Any procedures in pregnancy such as cervical stitch or sampling of amniotic fluid
- After having a miscarriage or a D&C (Dilation & Curettage is a surgical procedure to remove tissue from the womb)
- Premature rupture of membranes (your waters break long before your baby is due)
- Prolonged rupture of membranes – if your waters break more than 18 hours before your baby is born
- If you develop a urine infection (UTI)
- If your baby was born prematurely/early (before its due date)
- After you have had your baby – this is the most common time for serious infection (septic illness) to develop; especially if you had your baby by caesarean section/by forceps or vacuum delivery/or if you had a third degree tear (large tear to your perineum)
- Retained tissues after birth
- Breast infection leading to severe infection and abscess.
What can increase your risk of developing sepsis?
- Very overweight (obese)
- Diabetes
- Surgery within the last six weeks (including caesarean section)
- Having a weakened immune system
- Taking long term steroids
- Having, or recently had, treatment for cancer
- Heart, lung, liver and kidney disease (including conditions that you had pre-pregnancy).
When should I contact the midwife or doctor?
You should contact your GP or the maternity unit immediately if you are worried, unwell and/or if you notice any of the following:
- Sore throat and/or chesty cough;
- Urinary tract infections, pain/burning on passing urine or not passing urine in a day;
- Genital tract infection (vaginal/uterine infection) leading to vaginal discharge which may be foul smelling and/or an unusual change in colour;
- Abdominal pain that does not seem to be getting better;
- Chills, flu type symptoms;
- Diarrhoea;
- Sudden increase in postnatal vaginal bleeding (after your baby is born);
- Lumpy, red, painful, hot breasts;
- History of recent sore throat or prolonged (household) contact with family members with known streptococcal infections (pharyngitis, impetigo, cellulitis);
- A headache, neck stiffness, being unable to look at lights. Pain in the back after having an epidural or spinal pain relief;
- Swollen legs, red or painful calves;
- Pain, redness or, discharge from the place in your skin where a line or cannula was put in.
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the following: Telephone Triage – 01482 311750
For more information: UK Sepsis Trust at www.sepsistrust.org

