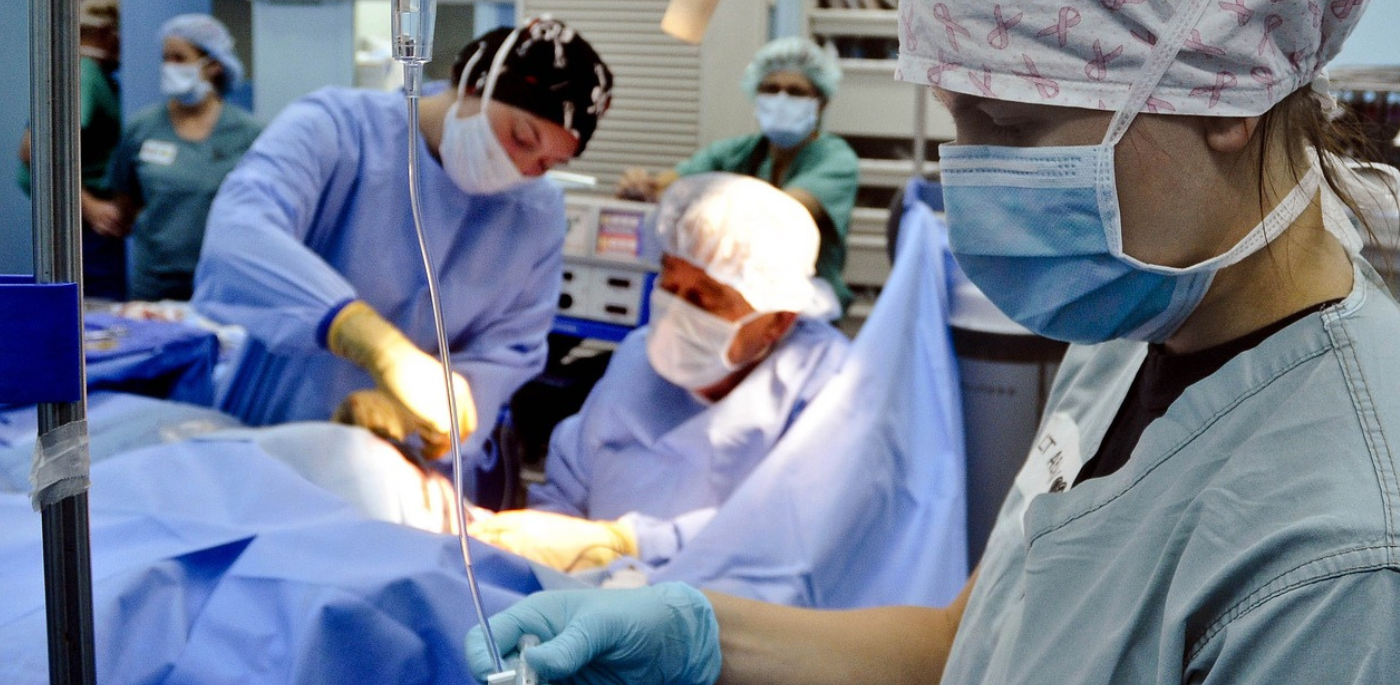
High levels of microplastics have been found in surgical environments in a landmark study.
A team at the University of Hull analysed microplastic levels in both the operating theatre and anaesthetic room, in cardiothoracic surgeries.
The study is the latest in a series of ground-breaking microplastics research from the University of Hull, Hull York Medical School and Hull University Teaching Hospitals NHS Trust.
Researchers discovered an average of 5,000 microplastics per metre squared when the theatre was in use, almost three times the amount found in our homes.
In addition, the anaesthetic room showed average levels of microplastics to be 500 per metre squared when in use.
Both settings had no microplastics settling out from the air when not in use.
Professor Jeanette Rotchell, Professor of Environmental Toxicology at the University of Hull, said: “You can imagine that during a cardiothoracic operation, which may last as long as eight hours, there will be a lot of people, utensils and consumable items. These items are all wrapped in plastic and this is contributing to all those particles in the operating room.
“It is a very dense environment for plastic particles to be introduced into the surrounding air. “
“The types of microplastic particles identified relate to common plastic wrapping materials.”
The majority of microplastic is PET – which would co-incide with blister packs, and polypropylene which may come from surgical gowns, hairnets and drapes for patients.
This study is the latest by the team in Hull which has already reported microplastics in abundance in outdoor and indoor environments and also in human lungs.
Other studies have also detected microplastics in the colon and blood, but until now, no studies have quantified microplastic levels in a hospital environment.
The study in surgical environments captured atmospheric microplastics for 12 hours per day in both operating theatres and anaesthetic rooms for seven days, on both working and non-working days; findings which will be replicated in surgical theatres throughout the country.
Professor Rotchell, said: “Although we know microplastics are in the air in a variety of settings, we can’t yet say what the consequences are or whether microplastics are harmful to health. Researchers have yet to establish this. “
“We do know that microplastics cause immune response type reactions such as inflammation in cell or tissue-based experiments. This study also highlights another route of exposure that differs from either inhalation or ingestion via our diet. In knowing the numbers and characteristics of the microplastics found in this study, we can now conduct more realistic cell type experiments to establish possible health impacts.”
Dr Daniel Field, lead investigator, said: “The invention of plastics was revolutionary for the surgical environment. “The fact you can vacuum pack equipment provides minimal risk to the patient and as doctors, our sole duty is to protect patients.”
“The amount of plastic used in operating theatres across Europe is astoundingly high – you can’t ignore it. We are producing a lot of plastic – much of it sterile, single use plastic and you can use 10-20 of these in a single operation just to take out a section of the lung, for example.
“While we do not yet know the actual health impacts of microplastics, if any, single use plastic is essential for the NHS that we see today. But that isn’t to say the NHS isn’t moving forward with goals and schemes in order to limit single use plastics elsewhere.”
Professor Mahmoud Loubani, co-author and a Consultant Cardiothoracic Surgeon at Hull University Teaching Hospitals NHS Trust involved in the study, found the results particularly interesting: “The environments in which we undertook our research are typical of most NHS operating theatres and anaesthetic rooms across the country, so we are confident in saying our findings will also be applicable to most if not all other clinical settings, locally and nationally, where major surgery is carried out.
“The NHS has moved to use a lot of single use instruments and equipment in surgery in the last 20 years which have improved our technical capabilities however this happened at the cost of increasing microplastics in the theatre environment.
“We have to consider ways of packaging the instruments as well as ways to open them that reduces the release of microplastics in the theatre environment.”
Hull University Teaching Hospitals NHS Trust has a growing reputation as a pioneer of innovative environmental healthcare practices and is one of the leading organisations in the NHS in the drive to reduce carbon emissions. The Trust has significantly reduced its use of carbon polluting anaesthetic gases in recent years and Castle Hill Hospital is the only facility of its size in Europe to be powered by solar energy.
The microplastics in surgical environments study was published in the Journal Environment International: