They’re always on hand to support the health and wellbeing of hospital staff, but nothing could have prepared Hull University Teaching Hospitals NHS Trust’s occupational health team for the arrival of COVID-19.
The 16-strong team is well versed in responding to crises and outbreaks, but the speed at which the pandemic was evolving and the resulting demands placed on the team were completely unprecedented.
Carole Hunter, Head of Occupational Heath for Hull University Teaching Hospitals NHS Trust says:
“The COVID-19 situation moved extremely quickly, and to be quite honest, the team has never seen anything like this.
“We initially started with the odd call from staff members and managers here and there, asking about how to report sickness or asking what to do if they had their own health concerns.
“This quickly escalated as the scale of the global pandemic became clear, and the situation became all the more real once we’d had our first COVID-19 positive patients at Castle Hill Hospital; the first patients to test positive in the country, in fact.
“Within the space of five weeks, the occupational health team took over 1,000 calls from hospital staff concerned about the implications of the virus for themselves, their patients, their family and their clinical practice. Such was the demand for advice and information, that with support from our infectious diseases team, we had to become COVID experts overnight. We had to keep on top of national guidance and advice that was coming out, be familiar with specific advice for employers and at-risk groups, and work with our own in-house experts in infectious diseases and tissue viability to develop our own guidance for staff as well.
“At the same time as responding to the incoming queries, there was a huge role for the team in ensuring our hospitals could be staffed appropriately to meet the potential demands of COVID-19. Initiatives to encourage retired NHS workers back into clinical practice, for example, had to be carried out at pace, and health checks for new starters which would ordinarily take three days to complete were being turned around within 24 hours.
“For those already employed by the trust, occupational health input has been a crucial part of the decision-making process when it comes to staff redeployment. Hundreds of clinical and non-clinical employees have relocated to work in other areas over the last couple of months, either to support areas of greater clinical need such as our COVID wards, or away from high risk areas if staff members are deemed to be at higher risk from the virus themselves. This too has been a huge undertaking for the team but crucial to our workforce planning, and to ensuring our hospitals could have the right people with the right skills in the right place at the right time.
“Because the situation is like nothing many of us have seen before, there will be a psychological toll on some staff. At the moment, many people are just getting on and responding to what’s asked of them, so the enormity of the situation or how they feel about what they’ve seen in recent weeks may affect them further down the line. Be it now or in the future, we are working closely with a team of psychologists, organisational development and the trust’s chaplaincy service to ensure staff have access to psychological support. Sometimes this can be just a chat and an opportunity to express their frustrations from the day at one of the regular drop-in sessions, but where any on-going or longer term support might be needed, it’s our role to ensure employees can continue to access that.
“We’ve also been ensuring staff can access advice and support in relation to skincare issues. As a result of more regular hand washing, more frequent use of hand sanitisers and for some staff, the need to wear more robust face masks and other PPE, some staff have experienced quite severe skin problems such as cracked and bleeding hands and sores on the face. Working with the tissue viability nurses, we’ve been able to develop and offer advice to staff to minimise these issues and provide creams and other products to try and ease any discomfort they may be experiencing. These are unfortunate side effects of practices which are necessary to protect people and save lives.
“As far as coronavirus is concerned, we’re by no means out of the woods yet, and the need to protect our staff from COVID-19 and to limit the spread of the virus will continue to form part of our plans and considerations across the organisation for many months to come.
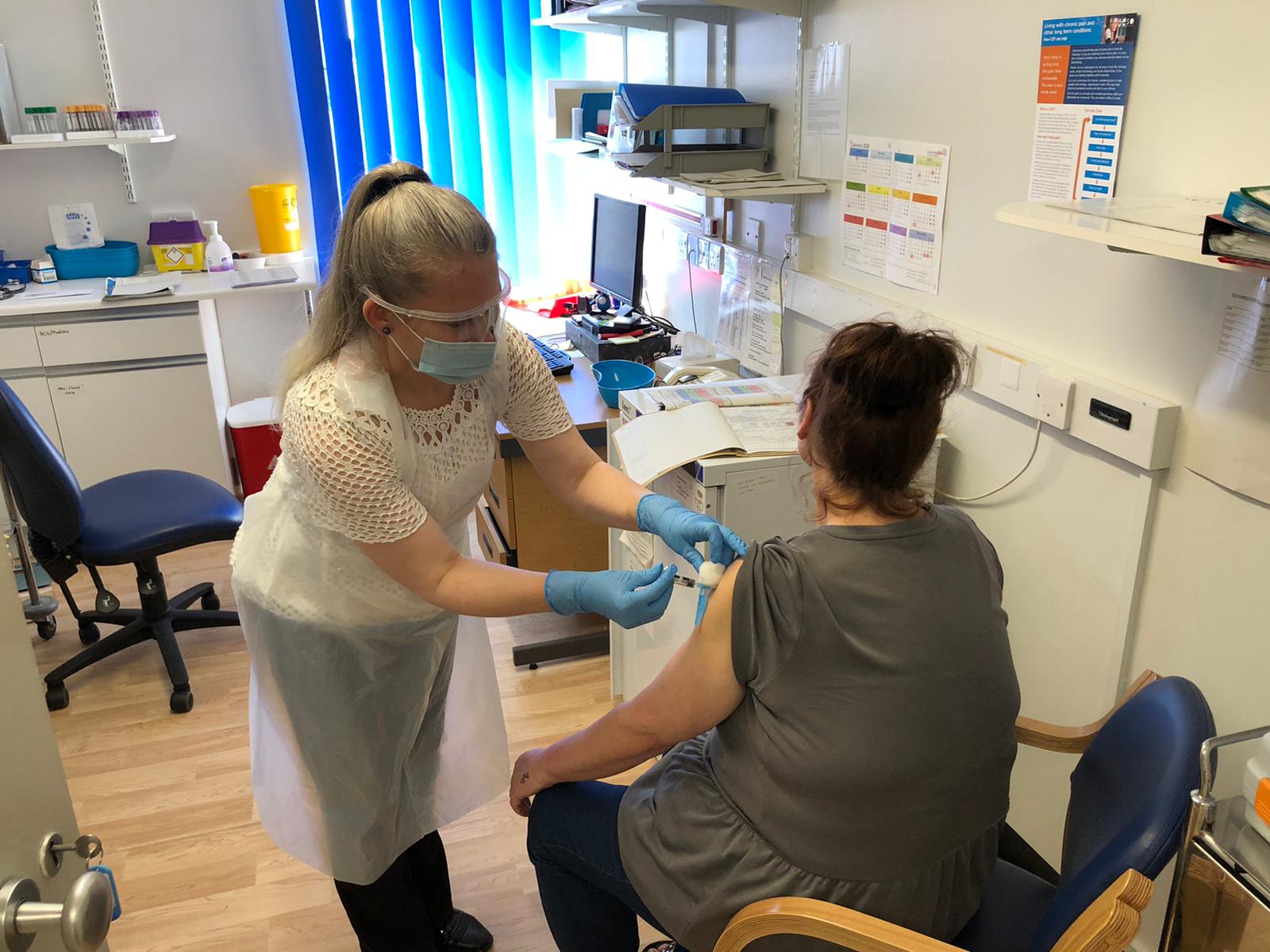
“At this time of year, for example, the occupational health team would normally start planning the delivery of seasonal flu vaccinations for staff. Hull is one of the best performing NHS trusts in the country for flu jab uptake, with 83% of staff involved in delivering frontline care vaccinated last winter, but our approach will be forced to change because of COVID-19 this year. Gone are the usual large scale drop-in sessions, and instead we’ll be looking to train more vaccinators within individual teams and departments to deliver this essential protection this coming winter.
“The impact of coronavirus is being felt in all parts of our hospitals and by everyone in it, but certainly as far as my team is concerned, they’ve taken it all in their stride and I’m really proud of how they’ve stepped up to the challenge. All nine of our occupational health nurses have rolled up their sleeves and just got on with the job, while the admin team have been fantastic in communicating with staff and keeping everything running smoothly.
“We’ve had members of our own team affected by coronavirus, we’ve seen staff in desperate need of help, and we’ve met ourselves coming backwards at times, but everyone is in the same situation. The most we can do is to protect our staff and safeguard their health and well-being, and in doing so, we give our patients the best possible chance of beating coronavirus too.”

