- Reference Number: HEY1622/2026
- Departments: Physiotherapy
- Last Updated: 30 April 2026
Factsheet for Patients
Introduction
We have written this leaflet to give you more information about vestibular rehabilitation. It explains what vestibular rehabilitation is, what it involves and how it can help with your recovery. We hope it will help answer some of the questions you may have. It is not intended to replace discussion between you and the therapy team. If you have further questions or concerns, please discuss this with a member of the therapy team.
What is the Vestibular System?
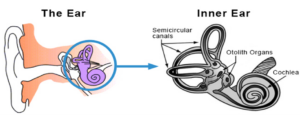
The vestibular system is in the inner ears, and it is made up of:
- The semicircular canals, which detect when your head moves in any direction.
- The otolith organs, which sense changes in head position and speed, such as when a car speeds up or a lift starts to move
These two areas send information to the balance system in your brain. The balance system also receives information from your eyes (visual system) and sensors in your muscles and joints (proprioceptive system). Your body uses all this information to stay balanced.
Dizziness, Imbalance and Vertigo
If one of the systems in your eyes, ears or rest of your body stops working or gets damaged, the brain may not receive enough information for the balance system to work properly. This can cause dizziness, vertigo (a feeling of movement or the world moving around you) and off balance.
- Dizziness can mean:
- A spinning sensation
- A movement sensation
- A falling sensation
- Light-headedness
- A general off-balance feeling
What is Vestibular Rehabilitation?
If the vestibular system in your ears stops working properly or is damaged, your brain can learn to adapt to the new messages it receives from the injured system, if you carry on completing your usual daily activities. Vestibular rehabilitation can help speed up this process. We will provide you with your own exercise programme to complete at home.
Will Vestibular Rehabilitation work for me?
Most people who complete their exercise programme see an improvement in their symptoms. Occasionally other interventions may be necessary.
How quickly will I see results?
You may notice an improvement in your symptoms within six weeks of performing your exercises regularly. The biggest improvement in your symptoms will usually occur within the first six months.
It is normal to feel worse when you first begin your exercise programme. If you continue with your exercises these symptoms should lessen.
How regularly should I complete my exercises?
We recommend that you complete your exercises three times a day, if possible, you may find it helpful to complete them at specific times each day.
It is important that you complete your exercises this often.
How difficult should my exercises feel?
Your vestibular rehabilitation exercises are supposed to make you experience some mild symptoms. It is important however, that your symptoms do not become too bad and stop you continuing with your normal day after exercising. If your exercises do not produce some symptoms, they are unlikely to work. By repeating movements that trigger dizziness or imbalance, starting gently and then making them harder, it can improve your tolerance and ability to do them.
Always ensure you challenge your balance in a safe way.
What should I do when my exercises become easier?
You should find that over time your exercises start to become easier. You can then challenge yourself further by:
- Increasing the speed of your exercise
- Increasing the number of repetitions
- Altering your position (if you have been completing your exercises sitting down, try standing up, or if you have been standing with a wide stance, try bringing your feet closer together)
- Changing what you look when exercising (e.g. if you have been advised to use a target for your exercises, try putting it on a busy background, such as a checkerboard, wrapping paper or patterned wallpaper)
Your vestibular therapy team will be able to help you adapt your exercises.
What else can I do to help my recovery?
Keep active
It is important that you keep active. Performing some form of exercise every day e.g. a short walk or some housework, will help to speed up your recovery.
Try to return to your normal movements and activities. We tend to reduce our movements e.g. keeping our head still, to stop us feeling dizzy or unsteady, but it is good to keep moving. It lets our brain experience the information it is struggling to understand to help it re-learn how to process the information.
Relax
It is important to maintain a good life balance during your recovery. Make sure you take time to relax and do the things you enjoy. You may want to look into meditation and mindfulness (an awareness of ourselves and the world around us) to help you to relax and feel more in control of your symptoms. This can be particularly useful if you have been suffering from anxiety, which is common in people experiencing vestibular problems.
There are apps available which you may find useful for meditation and mindfulness.
Consider your medications
You may have been prescribed medication to help reduce your dizziness and associated symptoms. Some can limit your rehabilitation and in discussion with your doctor it may be appropriate to stop or adjust your medication to help your recovery.
Pace yourself
Try not to push yourself too fast during your recovery. Remain patient and avoid pushing yourself so far that you need to go to bed to recover.
Think about breaking a difficult activity down into smaller parts and then slowly build up to completing it in full. This will help your confidence.
Contact Us
If you have any questions or concerns, please contact us.
Vestibular Rehabilitation Physiotherapy
Therapy Centre
Castle Hill Hospital
Castle Rd,
Cottingham
HU16 5JQ
Opening hours: Monday to Friday, 8.00am to 4.00pm
In the event you need to leave a message when you call (voicemails are checked regularly), please leave the following information:
- Your full name and date of birth
- Your hospital number and/or NHS number – if known
- A telephone number where we can call you between 8am and 4pm
Your feedback matters to us…
To ensure we deliver a safe and quality service and to help us understand the experience you have of the care you receive from our staff we would value your thoughts about the service you received.
You may be contacted as part of our quality assurance programme which is where we visit our teams and staff and talk to them about the care they provide to our patients or at any time during or after you have needed our services.
To collect this feedback, we would contact you using the registered telephone number we hold in your care record. This feedback will be strictly anonymous and whilst we will share the feedback as part of the process, we will not share any details which may identify you.
We will never ask you any personal questions about your health during these telephone calls.
If you do not wish to speak to us, please say this when we call, we do not want you to feel pressured.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.
