- Reference Number: HEY1618/2025
- Departments: Cardiac Surgery, Physiotherapy
- Last Updated: 31 October 2025
Introduction
This leaflet has been produced to give you general information about your upcoming surgery at Castle Hill Hospital. Most of your questions should be answered by this leaflet. It is not intended to replace the discussion between you and your doctor, but may act as a starting point for discussion. If after reading it you have any concerns or require further explanation, please discuss this with a member of the healthcare team caring for you.
What will happen in surgery?
You have probably been troubled by some symptoms. Following discussion with your consultant they have advised you attend hospital for a procedure to be undertaken on your heart.
There are a wide range of heart surgeries performed here at Castle Hill Hospital by our surgical team. You will have discussed at your consultation what operation you are going to have and why.
We recommend visiting the British Heart Foundation’s website for more information on your condition and treatment you may be having.
On the British Heart Foundation website, click on ‘Information and Support’. From here there are a wide range of topics covered, including how your heart works, tests you may have had/are going to have, and a wide range of information on treatment from both a surgical and non-surgical approach.

Can there be any complications or risks?
Having surgery can treat your condition, improve your quality of life giving you more energy for everyday tasks, reduce how hard your heart needs to work, reduce the risk of developing other heart conditions, and improve your symptoms.
As with any operation, there are risks with the procedure. Your consultant will have discussed the risks specific to you during your consultation as these vary from one operation to another. Understanding the risks and complications can help you decide if surgery is the right option for you and what other management options may be available to you. You may find it useful to take a family member of friend with you to your appointments to offer support.
How do I prepare for my surgery?
Please read the information leaflet. Share the information it contains with your family (if you wish) so that they can be of help and support. There may be information they need to know, especially if they are taking care of you following this examination.
Prior to your surgery it is important for you to attend all your appointments at hospital and with your GP. This will allow the medical team to prepare what they need to take into account prior to and after your surgery to help your recovery go as smoothly as possible. This will include a pre-assessment clinic where nurses and doctors will carry out tests, check your medical history, and address any concerns or questions you may have.
In the lead-up to your surgery, you will be asked not to eat or drink for a period of time in hospital. You may also be asked to adjust your medications – this will be advised by the medical team if required.
When packing for your hospital stay, we advise you bring comfortable, loose-fitting clothes, toiletries, regular medications in their original packaging, and suitable footwear. Remember smaller items like glasses, hearing aids, and dentures if you have them. Avoid bringing valuables or large amounts of money.
Try and get plenty of rest before admission and follow any instructions given by your medical team. Being prepared and well-informed can make a big difference to your peace of mind prior to surgery, and to your recovery.
What will happen?
On the day of your surgery, please attend ward 27 in the Centre for Cardiology and Cardiothoracic Surgery. You will be met by the medical team who will admit you to the ward and show you to your bed. You will be looked after by our nurses and doctors in the lead-up to your surgery, until you are ready to be taken down to theatre with your surgeon and their team. They will be responsible for looking after you during your operation. You will be under a general anaesthetic throughout your operation, closely monitored by the anaesthetics team. Following the completion of your operation you will be taken to our Intensive Care Unit, followed by ward 27 where you will spend most of your time recovering, initially in the high observation bay. This is also where you will be discharged from hospital.
What happens afterwards?
Wounds
Chest Incision
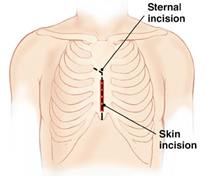
Following your operation, it is likely you will have a wound down the middle of your chest, called a sternotomy. Wires are used to join the breastbone back together again after your surgery which rarely need to be removed. You may feel grinding of the bone as it heals back together again, this may feel strange but is normal.
If you experience any ‘clicking’ of the bones this should be reported to your nurse or doctor.
Following a sternotomy, avoid heavy lifting and pushing and pulling heavy items (greater than 4lbs/2Kg, the weight of a bag of sugar) with each arm as this can put unnecessary pressure through the healing site. If you normally walk using elbow crutches, we will find an alternative walking aid for you to use whilst you recover.
Leg Incision
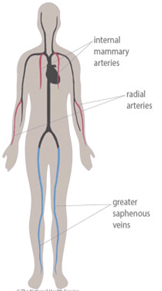
In some cases, your surgeon may use a vein from your leg to complete bypass grafts. Whilst recovering, this site can be uncomfortable but early movement of your leg will help to reduce stiffness and swelling. Physiotherapists on the ward will discuss exercises with you and any concerns you may have on the ward.
Forearm Incision
If the radial artery is used from your forearm, this site may be sore. Regular movement of your hand, fingers, forearm and elbow will help to loosen it again.
Please remember that pain around these areas is normal, and to be expected after your operation. It is important that you move regularly to help de-sensitise the pain and help the tissues heal and not become rigid and tight; this will only make movement more uncomfortable in the future. Continue to use pain relief at home as directed by the medical team to ensure you can do so.
Wound Care
Before you are discharged from hospital a nurse will check over your wounds and normally remove the dressings. Continue to keep your wounds clean when you return home. Soap and creams should be avoided on the wound area until it is fully healed; instead use clean fresh water. Speak with your nurse if you have any further questions.
Your wound will usually take 3 to 4 months to heal. Try to avoid picking at the wound as this can introduce infection and delay healing.
Continue to wear anti-embolic stockings during the day and night until you are seen at your follow-up appointment.
If there are any worrying concerns with your wounds, including redness, swelling, excessive discharge, new openings, or clicking/grinding consult your GP or contact the ward on Tel: 01482 469028.
Useful Post-Operative Recovery Information
It is normal after your surgery to experience aches and pains in your chest, back, shoulder, and neck due to stiffness of the muscles in and around these areas that have been stretched during surgery.
This is often worse in the morning but should start to ease with completion of your physiotherapy as discussed later in this booklet. It will gradually continue to improve as you go home. Continue to take regular pain relief as prescribed to ensure you can move comfortably and cough and clear secretions effectively. Taking pain relief in the morning and at night before bed should help you to get moving in the morning and sleep better at night. If your pain persists you can contact your GP to review your pain relief.
You may experience some of the following side effects, but they should improve with time:
- Sore throat and loss of voice.
- Hot and cold feelings/night sweats.
- Reduced appetite and changes in sense of smell and taste.
- Visual disturbances including blurred/spotted vision and hallucinations. We advise waiting 3 months before eye testing so that all disturbances from the operation have settled.
- Numbness or chest wall discomfort from your healing wound.
- Thumb numbness if your radial artery has been used for a graft.
- Leg swelling and numbness if a leg vein has been used for a graft. Continue to wear your anti-embolic stockings and try raising your legs slightly above hip height when resting. You may also experience an area of numbness around the base of the leg wound.
- Lack of concentration and memory loss. This can sometimes take 6 weeks to return to normal.
- Feeling anxious/tearful. It is normal after surgery to experience mixed emotions, including days where you feel great and days where you may feel irritable and tearful. This will improve with time as you become more confident. If you experience negative emotions for a long period of time, please contact your GP.
Physiotherapy After Your Operation
Discomfort:
Discomfort is normal after your operation but if your pain persists at a high level, please inform a member of staff so that further pain control can be prescribed. If you are in excessive amounts of pain, you will be reluctant to breathe deeply or move as often as we would like you to and this may delay your recovery.
Deep Breathing Exercises:
When on intensive care, you will be seen by one of our physiotherapists who will discuss deep breathing exercises with you. The purpose of completing deep breathing exercises is to help expand your lungs and move any secretions that may have built up which can cause chest infections.
We ask that you do 5 deep breaths at least every 30 mins after your operation
- Breathe as deeply as you can, hold for 3 seconds, then exhale slowly.
These may feel uncomfortable to do due to the tightness around your chest wound and drains but it is very important to persist. They will become easier the more you practise.
Coughing is also essential to help clear the secretions that will naturally build up in your lungs. It is safe to cough. You will be provided with regular pain relief and a rolled-up towel to help support your sternal wound when you cough.
Arm Exercises:
These need to be done to prevent your arms from becoming stiff and to start stretching your sternal wound. This will prevent the tissues from healing too tightly and will enable you to move normally.
Complete the following exercises 5 times each, 3 times a day, or as directed by your physiotherapist until your normal level of pain free movement is achieved.
- Circle your shoulders forwards and backwards slowly.
- Shrug your shoulders up and down slowly.
- Raise both arms out in front of you then up and above the head slowly.
- Raise the arms out to the side then up and above the head slowly.
- Place your hands behind your head then behind your back slowly.

Leg Exercises:
These encourage good circulation of blood around the body and help to prevent formation of clots. They also help start to prevent joint stiffness, especially if you have had a vein used from your leg. We advise you to complete these 5 times every hour.
- Wriggle toes.
- Circle your ankles in both directions.
- Paddle your feet up and down.
- When sitting in bed, push your knees down into the bed and tighten your quadriceps muscles, hold for 3 seconds then relax.
- Tense your buttock muscles, hold for 3 seconds then relax.
Avoid sitting with your legs crossed as this restricts blood flow.

Mobility:
Once safe to do so, you will sit out in your chair on intensive care. This helps to naturally exercise your heart and lungs again and improve the circulation in your legs. It is normal to experience some dizziness and the feeling of weak legs however this will pass with time. This may feel uncomfortable, and you may be anxious about moving so soon after your operation, but you will be closely monitored throughout and not pushed beyond what is safe for you.
Continuing Exercise At Home
Continuing to exercise at home is important in aiding your recovery from surgery for a variety of reasons:
- Strengthens the heart.
- Maintains a normal blood pressure.
- Increases confidence.
- Reduces cholesterol.
- Keeps bones and muscles strong.
- Mental benefits.
Walking is one of the safest forms of exercise following your hospital discharge until you have your 6 week consultant follow-up where you can discuss return to other activities such as golf, swimming, cycling, and others. Make sure to avoid exercise that causes excessive straining whilst your wounds are still healing.
Stop activities that cause of any of the following:
- Dizziness
- Heart palpitations
- Chest discomfort
- Sickness
- Cramps
- Extreme fatigue
Intensity:
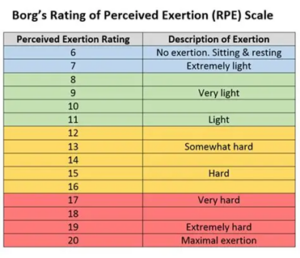
Walk at an intensity that feels comfortable but challenging for you, remember this will be different for everyone so try not to compare yourself to others.
The Rating of Perceived Exertion Scale is a good way of judging your exercise intensity.
11 to 13 is a good range to aim for.
We recommend you start with a consistently steady pace that feels comfortable until you can achieve a 30 minute walk, then you can start to increase the intensity by walking at a brisker pace or walking on slight inclines, and continuing to increase the time by 5 minutes when able.
You may find it helpful to walk with friends or family members whilst your confidence is improving.
If the weather outside is unsafe, you may find our indoor exercise programme useful. You can find these exercises near the back of this booklet, demonstrated by one of our physiotherapy assistants.
Hobbies
Additional activities can be started around 6 to 8 weeks after your operation, make sure to discuss these with your consultant at your follow-up appointment which the hospital will organise for you.
Some of our recommendations:
- Cycling – Start on flat ground or an exercise bike. Start on flat ground for short distances and gradually build up the distance and intensity.
- Swimming – Once your wound is fully healed start with small amount of comfortable strokes and build up the distance and intensity gradually.
- Golf – Start with gentle putting, then progress to short distance pitches, then gradually larger swings until you feel ready to play some shorter holes and eventually a full round.
- Dancing/Bowling/Fishing – Start gently and progress slowly when you feel able to.
- Jogging – Start on flat ground and slowly build up your pace, stride length and distance.
- Contact sports – Speak directly with your consultant.
- Gardening – Do not dig or push a lawnmower for 3 months.
Household Tasks
Household tasks are still safe to continue when you go home, please see our below precautions to consider.
| Activity | Precaution |
| Washing Up | Avoid lifting heavy pots that may be filled with water. |
| Dusting | None |
| Ironing | Do not lift heavy ironing board. |
| Vacuuming | Start with small areas. Do not lift a heavy vacuum up the stairs. |
| Making beds | Avoid for approximately 2 weeks when you return home. |
| Cooking | Avoid lifting heavy saucepans. |
Avoid lifting heavy weights and pushing or pulling on your car if it breaks down. Generally, avoid tasks that require you to ‘grunt’ with effort to complete them.
Driving
Obtain permission from your consultant at your 6 week follow up which the hospital will arrange for you. It Is important you can full turn the wheel and look in all your blind spots comfortable to be safe when driving. You must continue to wear your seatbelt; you can place a towel or cushion between your chest and belt if the belt is too uncomfortable.
You must inform your insurance company of your operation prior to driving again. You are not required to tell the DVLA unless you have recurrent angina, dizziness, or palpitations, or if your insurance company requests you to.
Group 2 License Holders
You must inform the DVLA of your medical condition and surgery. You won’t be able to drive for 6 weeks and must reapply for your license once safe to do so.
Sleeping
Your bed does not need to be brought downstairs. Once you are ready to be discharged from physiotherapy, we will discuss your safety when completing stairs and may practise them in hospital before you leave. Sleep in a comfortable position at home but try to avoid lying on your front for 6 weeks. Sitting up slightly with pillows to support you may help with comfort initially, then you can slowly return to a normal position as comfort allows. It may take a while to get back into your normal sleeping pattern; this is normal as you readjust to life at home.
Sexual Intercourse
This can be resumed once you feel able to. Build up duration and intensity just as you would any other form of activity. Choose positions that feel safe for you and don’t cause discomfort around your wounds.
Return To Work
We recommend you speak with your consultant at your follow-up appointment, or with your GP regarding return to work. As with other activity, build up gradually with a phased return to work/reduced hours if possible.
Holidays
It is recommended to avoid going away on holiday for around 6 to 8 weeks until you have had your follow-up appointment with your consultant. If you have a holiday planned before this time you should speak to your consultant or GP. We recommend you to not travel until your wounds have healed and any symptoms from your operation have healed.
During a flight we recommend you walk regularly and perform simple leg exercises to help blood flow and prevent clots in the legs. For the same reasons, during long car journey stop regularly to walk around and stretch. You can find these in our recommended exercises at the end of this booklet.
It is advisable to keep your wounds covered from the direct sun or use a good protective suncream for 6 months after your surgery to stop the healing skin from burning. Some medications may also affect your sensitivity to the sun, particularly amiodarone, speak to your GP regarding managing this.
Alcohol
Unless otherwise advised by a member of the medical team, approximately 1 or 2 units a day is okay.

Diet
For information on diet, we recommend you visit the British Heart Foundation’s website where a wide variety of topics are covered that would be too much to cover in this booklet alone. There you can find information on:
- Simple tips to make healthier food choices.
- How to maintain a balanced diet.
- Portion size guides.
- Weight loss advice.
Going Home & Outpatient Follow-Up
Once home, try to limit your visitors to allow you to rest properly, 2 a day is sufficient. You may contact your GP to inform them of your surgery and organise repeat prescriptions; the hospital will contact your GP with a hospital summary when discharged.
You will receive an outpatient hospital follow-up appointment for around 6 weeks after your operation. Please contact the department using the contact number on your letter if the date/time is unsuitable. If you do not receive a follow-up appointment, please contact your consultant’s secretary.
At Home Exercises
See below images and explanations of simple exercises you can try at home if you wish to continue to build your strength, balance and confidence. If you feel these exercises may be too easy/challenging for you, speak to a member of our physiotherapy team who can advise you on alternatives. You will also receive a letter to attend cardiac and pulmonary rehab, who will also be able to advise you on activity modification and exercise following your surgery should you wish to attend.
Here are some exercises you can complete at home if you wish to:

Marching on the spot – Hold onto something if needed for your balance. Stand tall and lift your knees one at a time as if marching. Maintain a steady rhythm.
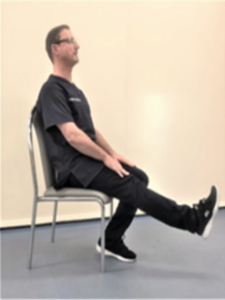
Leg extension – Sit in a sturdy chair, feet flat on the floor. Straighten one leg out in front of you until your leg is straight. Hold for a second, then slowly lower back to the floor. Repeat on the other leg.

Heel raises – Hold onto something for your balance. Slowly lift your heels off the floor, rising onto your toes, then lower back down to the floor.

Mini squats – Stand tall holding onto a support if needed. Bend your knees slightly until you reach a perched position, then push back into a standing position with your legs.

Hamstring curl – Stand tall holding onto a support. Bend one knee to bring your heel close to your bottom then lower back down to the floor. Repeat with the other leg.

Step-ups – Hold a handrail for support. Step up onto a step with 1 foot, then bring the other up to join it. Step back down with one foot followed by the other. Repeat at a steady pace.
Cardiac Surgery Recovery: 6 Week Walking Activity Tracker
Use this tracker to record your daily walks as you recover from heart surgery. Aim to gradually increase your walking time and distance each week. Stop and rest if you feel chest pain, dizziness, or shortness of breath. Bring this tracker to your follow-up appointments.
How To Use:
- Record each activity and how you felt
- Aim for small, steady progress each
- Walk on safe, flat routes and wear comfortable
- Stay hydrated and walk with someone if
Tips For Safe Walking:
- Warm up and cool down
- Avoid steep hills or uneven
- Walk with someone if
- Wear comfortable
- Stay
Week 1
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Week 2
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Week 3
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Week 4
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Week 5
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Week 6
| Day | Activity 1 | Activity 2 | Activity 3 | Notes |
| Monday | ||||
| Tuesday | ||||
| Wednesday | ||||
| Thursday | ||||
| Friday | ||||
| Saturday | ||||
| Sunday |
Should you require further advice on the issues contained in this leaflet, please do not hesitate to contact the Department of Cardiothoracic Surgery on Tel: 01482 469028.
General Advice and Consent
Most of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion with the healthcare team.
Consent to treatment
Before any doctor, nurse or therapist examines or treats you, they must seek your consent or permission. In order to make a decision, you need to have information from health professionals about the treatment or investigation which is being offered to you. You should always ask them more questions if you do not understand or if you want more information.
The information you receive should be about your condition, the alternatives available to you, and whether it carries risks as well as the benefits. What is important is that your consent is genuine or valid. That means:
- you must be able to give your consent
- you must be given enough information to enable you to make a decision
- you must be acting under your own free will and not under the strong influence of another person
Information about you
We collect and use your information to provide you with care and treatment. As part of your care, information about you will be shared between members of a healthcare team, some of whom you may not meet. Your information may also be used to help train staff, to check the quality of our care, to manage and plan the health service, and to help with research. Wherever possible we use anonymous data.
We may pass on relevant information to other health organisations that provide you with care. All information is treated as strictly confidential and is not given to anyone who does not need it. If you have any concerns please ask your doctor, or the person caring for you.
Under the General Data Protection Regulation and the Data Protection Act 2018 we are responsible for maintaining the confidentiality of any information we hold about you. For further information visit the following page: Confidential Information about You.
If you or your carer needs information about your health and wellbeing and about your care and treatment in a different format, such as large print, braille or audio, due to disability, impairment or sensory loss, please advise a member of staff and this can be arranged.

